No Medicaid, No Medicare.
Our Tampa Facility
Pool Next to Private Rooms
Pool Next to Private Rooms
Private Room Overlooking Pool
Private Rooms Featuring Private Bathroom
Relax and take a break at the outside snack and lounge area
Breaks and free time can be enjoyed in the outdoor common area featuring picnic tables and lounge chairs
Entrance to Outdoor Lounge Area and New Rec. Center
Outdoor Seating and Lounge Area
Boxing Ring and Training Area
Full Range of Exercise Equipment Featuring Boxing Ring
Front Door and Entrance Area
Lobby and Reception Area
Our Fort Myers Residential Campus, Offering all Levels-of-Care
Entrance to Main Lobby and Reception Area
Lobby and Welcome Area
Swimming Pool
Updated Private Rooms
Accomodations: Each Home Featuring Private Rooms
Amenities Including Gazebos, Walking Paths, and More
Spa and Therapy Rooms
Yoga Room
Our Hyde Park (Central Tampa) Location, Day-Night/IOP Levels of Care (Transitioning)
Aerial View of our Facility Located in Close Proximity to Downtown
Entrance to Facility
Entry to Home-Style Living
Renovated Private Rooms
Lounge/Living Room Area and Common Space
Mission Statement - Raising Industry Standards
WhiteSands Treatment Center was founded in 2014 with the overarching philosophy that it was time to raise industry standards with respect to the quality of treatment, comfortability of patients, and increased rates of long-term sobriety. We recognized that national relapse rates were abysmal and treatment protocols have remained stagnant for many years. Our founders, CEO Garry Jonas and COO Joseph Ducey had a vision to create a treatment program that stood well above its competitors and that treated patients as individuals while also providing many of the comforts of their home environments.
WhiteSands hired accomplished Clinical Director, Dr. Lyndsay Henry, as the centerpiece for a strong clinical team. Dr. Henry accepted the position with the condition that ownership allow the clinical and medical teams to operate unrestrained regardless of expense to create the most effective treatment program. Dr. Henry, Mr. Jonas, and Mr. Ducey carefully selected a specialized management team and began analyzing what innovations could be developed to raise the bar within their treatment facility.
Providing Truly Individualized Treatment
- We have been on a mission to develop the most comprehensive and individualized treatment program
- We believe that one-on-one care should be expanded within the treatment experience
- By focusing on individualizing the treatment experience, we are finding that patients can better understand and address the issues underlying their addictions
- It is our goal to help those we serve to gain a better awareness of underlying emotional challenges
At WhiteSands, we begin to help patients address the underlying issues from the very first day they start their journey with us. Within the first week of treatment, each patient meets with our medical director, clinical director, psychiatrist, and individual therapist multiple times. As a team, each patient’s needs are carefully reviewed to determine what the best course of treatment will be.This includes working with each patient to help them establish goals for individual therapy, selecting therapy group options, and their individualized need for medical treatment. Each patient will have 4-5 individual and/or family therapy sessions per week. This requires WhiteSands to have a larger number of qualified clinical staff as part of its treatment team.
At WhiteSands, we believe in true individualized treatment and implement this in a variety of areas. We do not believe in moving patients like cattle from one group to another where everyone is following the same treatment program regardless of background or circumstances. From the conception of WhiteSands to present, we have been on a mission to develop the most comprehensive and individualized treatment program.
It has been the philosophy of WhiteSands that too many treatment centers focus on treatment as a group endeavor. While primarily focusing on group treatment may be easier and less expensive, we believe that one-on-one care should be expanded within the treatment experience.
Most treatment centers divide patients into one or two tracks with limited options. While this may meet the needs for some in treatment, we have found that most patients are looking for more options to choose from in meeting their personalized needs. We believe when programs are not more individualized, there may be a higher probability patients will become disengaged from the treatment experience, leading to poorer outcomes in achieving and maintaining sobriety. By focusing on individualizing the treatment experience, we are finding that patients are able to better understand and address the issues underlying their addictions. At WhiteSands, we strongly oppose the one-size-fits-all approach and have designed our programs to meet everyone’s individual needs.
We all know the abysmal statistics on relapse rates following completion of treatment, and our industry needs to continue to strive to improve these outcomes. At WhiteSands, we believe the heart of improving outcomes is getting to the underlying issues of why someone uses substances. Why are they self-medicating with drugs and alcohol? A person can be physically detoxed from the substance in 7-10 days, but the mental withdrawal and obsession lasts much longer. At WhiteSands, we want to focus on what is at the heart of the mental component of addiction.
Determining the underlying issues and the mental component of addiction takes intensive one-on-one therapy and having a broad menu of groups to choose from that can address any underlying issues. At WhiteSands, it is our goal to help those we serve gain a better awareness of underlying emotional challenges such as depression and anxiety, how to cope with past traumatic experiences, how to cope with family dynamics, and how to cope with situational stressors present in the home/work/social environment. We believe that we cannot get to the underlying issues if we limit the treatment modalities offered and if the group sizes are too large. We strive to hire staff with diverse backgrounds and specialties, so that we can assign a patient to the therapist best able to cope with their needs.
Replacing Harmful Addictive Behaviors with Healthy Habits
- We support patients by helping them create healthy habits, which can become a new part of their daily routine
- We have worked hard to create a program that encourages patients to be mentally and physically active during the time they are not in active individual or group therapy
At WhiteSands, we recognize that humans are by nature creatures of habit that can be prone to addiction and obsessive behaviors. Individuals with addictive personalities are going to struggle with moderation in any area of their life. At WhiteSands, we first focus on the harmful addictive behavior that is leading them to enter treatment and has been destructive in their daily lives. We support patients by helping them create healthy habits, which can become a new part of their daily routine.We also help them avoid falling into the pitfall of other harmful addictive behaviors following completion of our treatment program. We address this by helping them examine other areas of life for potential addictive behaviors such as work, exercise, food, spending money, or sex addictions and creating a detailed relapse prevention plan that monitors each of these other areas of life prone to addiction.
Many treatment centers have patients being mentally and physically unchallenged throughout their treatment program. They are often either sitting in group sessions or chain smoking on a bench outside while experiencing increased anxiety and agitation as a result of that treatment experience. Although we do permit smoking and utilize group and individual therapy, we have worked hard to create a program that encourages patients to be mentally and physically active during the time they are not in active individual or group therapy. An individual in treatment for 4-6 weeks has the opportunity to not only address their addictive behaviors while also having the opportunity to spend time working on their physical health and general life management skills.
A Comfortable Guest Makes a Successful Patient
At WhiteSands we believe that patients should be comfortable and treated with dignity and respect at all times. Our CEO, Garry Jonas recognized that many treatment centers treat patients like cattle, moving them from one location to another in a group, with little recognition of the uncomfortableness and shame with which many patients struggle with, as they work on their issues. He recognized that the agitation and anxiety many experience was due to patients not being in the comfort of their own home. This led to the pioneering idea of designing a program with most of its therapy occurring during the hours of 8:30am-4:30pm and in the evenings, patients become guests. This schedule mimics the reality of many people returning to work and home. There are set hours each day for therapy and for relaxation.
We have all recognized that many patients enter treatment at their personal “rock bottom” and are often highly agitated and anxious. People do not enter treatment because their life is going great, their emotions are balanced, and they have healthy coping skills. Many people enter treatment following an intervention from family, friends, or an employer that have increased feelings of shame and anxiety. These feelings can increase throughout the treatment program experience, and for many, may lead to difficulty engaging in treatment or absorbing the information presented to them. While the patient is trying to deal with these challenging issues, treatment centers typically make it more difficult by limiting the patient’s comforts of home. Limiting these home comforts, such as no access to electronic devices, sharing a bedroom and bathroom, and being told what to do every minute of the day can all significantly increase the agitation and anxiety already present.
What Does ‘a Patient Becoming a Guest’ Mean?
At WhiteSands, we worked to create an environment with a hotel/resort like atmosphere. At 4:30 PM, after completing a full day of groups and individual therapy, patients are able to return to their private bedrooms and find their personal electronics (phones, tablets, laptops) waiting on their queen-sized beds. They are able to check in with family, friends or work, check emails or social media and process what they have learned that day in their personal sanctuary. They are able to have privacy watching television in their bedroom or engage in various activities on our campus.
From 4:30 PM - 10:30 PM, they can create their own schedule. Some people prefer to spend time in small groups playing volleyball, playing basketball, swimming, or playing board games while others prefer to read in their rooms, walk quietly around our property, or exercise in our large recreation center. We want each individual’s needs to be met during this time. They are able to eat healthy food prepared on our property either in their rooms or on their patios. Many choose to eat dinner with their families over video calls.
At WhiteSands, we believe that providing access to electronics offers a necessary degree of privacy and freedom, but we ensure this is done within a clinically supportive environment. Clinicians are on-site during these hours to process negative phone calls, confrontation by family members, or contact from unhealthy friends or family that may lead to cravings being triggered. We fully believe that if we were to limit access to electronics throughout the entirety of a treatment stay, individuals would be confronted with an overwhelming number of triggers once they return home. With allowing them access while in treatment, they are able to learn to process these triggers in a supportive environment where drugs and alcohol are not available.
At 10:30 PM (or earlier for those who prefer to go to sleep earlier), all devices are collected, and a period of self-reflection and reading is encouraged before turning in for the night. Life Skills reading is provided daily, and many take this time to complete reading assignments or journal. This allows them to enter treatment in a healthy and positive mindset the next day.
At WhiteSands, we truly believe that treating a patient like a guest after clinical hours teaches them that they deserve to experience healthy pleasures in life and learn to have fun while sober.
Our Unique Life Skills Program
- The Life Skills Program is centered around creating and maintaining a healthy and balanced routine in daily life
- Our Life Skills Program is first administered by the individual therapist and we provide 4-5 individual sessions per week
- The Life Skills Program is based on having balance throughout the day including sleeping well, eating well, and exercising
At WhiteSands, we encourage patients to focus on their health, general well-being, and organizational skills. To help them achieve this, we are proud to share that we have created a specific Life Skills Program to help each individual achieve this goal. The Life Skills Program is centered around creating and maintaining a healthy and balanced routine in daily life. We have witnessed great success in not only helping individuals maintain sobriety but also in helping them implement changes and improve their entire lives. The key to relapse prevention is sending them home with new healthy living habits.
Our Life Skills Program is first administered by the individual therapist. We provide 4-5 individual sessions per week, with one focused entirely on the Life Skills Program. Each patient is also assigned a Life Skills Guide who helps them execute their personal Life Skills Program on a day-to-day, hour by hour basis. Each patient has the option to be assigned a personal trainer and nutritionist throughout their treatment stay. An important component of the Life Skills Program is learning to begin the day by writing out a detailed plan of what the day will look like including meals, exercise, therapy, family contact, and increasing sober support. For many individuals in early recovery, understanding how to not give into one’s own impulses is a significant issue that needs to be addressed. Creating the daily schedule greatly decreases decisions made with poor impulses. This becomes an important component of creating healthy habits via visualization and execution.
Throughout our Life Skills Program, we want to teach patients to develop healthy time-management skills, to set healthy and achievable goals, to achieve balance in their work, personal life, health, and recovery, and to monitor their mood, behaviors, and accomplishments closely so they are aware when they are veering off track.
The Life Skills Program is based on having balance throughout the day including sleeping well, eating well, exercising, working smart by being organized, and has the overall philosophy of “plan your work and then work your plan.” During the Day/Night (PHP) phase of treatment, and in collaboration with the patient, the individual therapist and Life Skills Guide will work together to focus on what each individual’s routine will look like once they return home. This is critical to relapse prevention as many people do well within the structured environment of treatment but then return to a chaotic environment and relapse rapidly. We want to work with each patient to transfer the healthy habits they learn in treatment to their home life.
WhiteSands Recovery and Wellness
- Patients are meeting daily with Life Skills Guides and learning new time management techniques, scheduling techniques, and how to create Self-Management and Recovery Training
- These Life Skills Guides will assist in helping patients stay on track
- Participants in WhiteSands Recovery and Wellness will additionally have access to a 24-hour hotline they can call anytime they are struggling
- We believe it is our duty to assist patients in staying sober even after they have completed treatment
- WhiteSands Recovery and Wellness was created to allow us to continue “monitoring” the behaviors of patients long after they are out of our residential levels of care
- We have learned the benefits of virtual connection that can allow patients to continue to participate with WhiteSands once they return home
WhiteSands Recovery and Wellness is an extension of our Life Skills program discussed in previous sections. While in detox, residential, and day/night (PHP) levels of care, patients are meeting daily with Life Skills Guides and learning new time management techniques, scheduling techniques, and how to create Self-Management and Recovery Training (”SMART”) Goals from their therapists. After completing these levels of care and returning to the “real world,” their Life Skills Guides will continue to follow-up with them daily and to ensure they are continuing to begin their day by writing out their daily schedule including meal plan, exercise plan, tasks to be completed, and time they need to be sleeping. Guides will be monitoring that patients are continuing to stick by the plan they created in inpatient treatment and will be available to discuss triggers or stressors that arise.
These Life Skills Guides will assist in helping patients stay on track and be able to rapidly support patients if they are showing signs for potential relapse. Guides will continue monitoring their daily behaviors for as long as necessary and will always be a source of continued support. This will also allow us to gather in depth data on the success rates of our program and identify any other treatment program needs which may be helpful in ensuring the best sobriety maintenance outcomes.
WhiteSands Recovery and Wellness will not only allow patients to maintain contact with us through their Life Skills Guides but will also allow them to continue seeing the same therapist, medical provider, and psychiatric provider via in person or telehealth (video) sessions. This allows them the unparalleled opportunity to continue to see providers they have begun trusting, who know their history, rather than having to begin to develop a relationship with someone new.
Additionally, participants in WhiteSands Recovery and Wellness will additionally have access to a 24-hour hotline they can call anytime they are struggling and that will be answered by individuals in recovery themselves. They will be able to virtually access multiple alumni and check-in meetings daily to have a safe place to process any events, feelings, or triggers amongst peers.
As they gain greater periods of sobriety, participants will be able to participate in KO Addiction’s quarterly boxing events where they will be celebrated for their achievements and be able to provide their experience, strength and hope to those early in a recovery journey. KO Addiction is a non-profit organization that works to highlight drug epidemic issues currently facing our nation, to engage our community to provide support for those issues, and empower individuals to force change.
Our overall goal at WhiteSands is to not only help people get sober and maintain long-term sobriety, while also helping assist them in achieving their full potential in life , whether in relationships, work, and in their overall health.To help patients take the skills they learned in our Life Skills Program into their daily lives, we will offer them the same Life Skills Guide they had in treatment so they remain connected with them once they return home. This is accomplished via daily virtual check-ins as well as in-person check-ins when feasible. We believe this will allow us to catch many “slips” before they happen. If a “slip” does occur, it can be caught early and then does not require further inpatient treatment that takes patients away from work and family again.
A long-term Life Skills Guide for each patient is a significant and costly undertaking that is unique to WhiteSands; however, we believe it is our duty to assist patients in staying sober even after they have completed treatment. At WhiteSands, we believe “once a patient, always a patient” and want them to stay part of our family. We believe our program will greatly decrease relapses from occurring, given our unique approach offering.
At WhiteSands, we believe preventing relapse can be brought to a whole new level. We know that we have successfully detoxed many patients and have witnessed them complete our program and graduate successfully. While many patients look and behave like new people by the end of their treatment program experiences, many of these same patients return to their home environments and quickly change back to old habits due to the lack of structure and support for their sobriety. Many treatment centers emphasize relapse prevention throughout the treatment stay but then leave patients to implement their plan and cope with the triggers which make them vulnerable to use again, when they return home on their own. We believe this can set them up for failure. We recognize that we needed to do more to assist our patients in maintaining long-term sobriety and reaching their highest life potential. Thus, we created the WhiteSands Recovery and Wellness Program.
Our CEO, Mr. Jonas, developed a tried-and-true credo that he has utilized to manage his business for many years. “People don’t do what you expect, they do what you inspect.” WhiteSands Recovery and Wellness was created to allow us to continue “monitoring” the behaviors of patients long after they are out of our residential levels of care. Through this challenging year of Covid-19, we have learned that we do not always need to be in physical proximity of doctors, therapists, and peers to be able to communicate and observe behaviors. We have learned the benefits of virtual connection that can allow patients to continue to participate with WhiteSands once they return home.
Flexible Lengths of Stay
- We have created a flexible 60-day program that combines inpatient and outpatient treatment stays
- Once a patient graduates from the 60-90 day inpatient and intensive outpatient program, they become a part of the WhiteSands Recovery Program which supports them in maintaining long-term sobriety
The overall philosophy and treatment program of WhiteSands is based on a 60-90 day treatment stay encompassing both inpatient and outpatient levels of care; however, we recognize that lengths of stay will vary, and some patients are only able to complete a 7-day stay due to various issues such as time away from home, cost, family obligations, work obligations, and insurance coverage.
Based on these considerations, we have created a flexible 60-day program that combines inpatient and outpatient treatment stays. For some patients, this means 7 days of detox and 53 days of intensive outpatient treatment, but the majority of our patients chose to stay in our 35-day inpatient program (comprised of detox, residential, and day/night (php) levels of care) followed by 25 to 55 days of intensive outpatient treatment where they can reside in their home or in a recovery residence.
It is important to note that once a patient graduates the 60-90 day inpatient and intensive outpatient program, they become a part of the WhiteSands Recovery Program which supports them in maintaining long-term sobriety with continued outpatient therapy and follow-ups with affiliated medical providers who are experienced in addiction treatment.
For the purpose of illustration, we will provide examples of what each level of care encompasses using average lengths of stay that have led to success. The actual course of treatment will always be based on medical necessity, doctor/therapist’s recommendations, and insurance and financial capabilities.

Levels of Care
At WhiteSands Treatment, all treatment services share common and key elements in providing comprehensive, individualized care for co-occurring disorders. These include having M.D., Ph.D. and Nursing level staff skilled in the diagnosis of psychopathology. All staff members are cross-trained to deal with addictions and substance-related disorders.
Detox Program
- The Detox Program generally lasts 5-10 days with our average length of stay being 7 days
- Each patient is met by an admissions coordinator and nurse who will ask basic questions, take vitals, and have a urinalysis completed
- The patient is then escorted to the comfort of their private bedroom
The Detox Program generally lasts 5-10 days with our average length of stay being 7 days. Detox begins at the point of admission. We strive to make our admissions process as comfortable and quick as possible. We recognize that entering treatment may be emotional and anxiety provoking and that many individuals are struggling with shame and embarrassment. Please click below to see the details of our admissions process and how we cater to the patient, the family, and any third party referring them to our program.
- At the point of arrival, each patient is met by an admissions coordinator and nurse. The nurse will ask basic questions, take vitals, and have a urinalysis completed to ensure and consult with appropriate medical professionals to confirm we are the right program for the patient.
- Once the nurse determines the patient is appropriate for admit, the patient signs a consent for treatment and other basic forms and then is escorted to the comfort of their private bedroom. The rest of the admissions process occurs in the bedroom to ensure privacy. Various departments can come and go as necessary, but the patient is able to remain in their room through this initial admission process.
- Each patient will have their belongings searched and inventoried by a behavioral health technician and will receive their belongings within a few hours.
- Extended slow tapers off of all mood and mind-altering substances. With the benefit of slow tapers, you are able to, but not mandated to attend group therapy from day 1. We understand there is an adjustment period for anyone entering treatment. Using a combination of controlled medications, our board certified Addictionologist will meet with you every day throughout the course of your detoxification, to both ensure you are as comfortable as possible, and make any necessary adjustments to your individualized protocol. Your safety and comfort are of the greatest importance to us through the detoxification process.
Note: Complete history and physical within the first 24 hours of admission to WhiteSands.
More Info on DetoxMedically Assisted Detox
- Offered at our Fort Myers and Plant City Locations
- Typical duration is 5-10 days
- Before participating in residential/inpatient treatment, many patients require a period of medically assisted detox where they are carefully weaned off of the substance of abuse. This takes place in a closely monitored environment where your comfort is of paramount concern to us.
- We utilize several medications for an extended taper, based on medical symptoms and history of use. With the benefit of slow tapers, you are able to, but not mandated to attend group therapy from day 1. We understand there is an adjustment period for anyone entering treatment.
- Patients are seen daily by our medical director (Board Certified Addictionologist) while on detox to ensure you are responding well to medications, and not experiencing withdrawal symptoms.
- Patients have a complete history and physical completed within 24 hours of admission as well as a complete psychiatric evaluation within 48 hours of admission.
- Patients will also be seen by their primary therapist within the first 48 hours to start a treatment plan and outline goals while in treatment.
- We employ 3 Addictionologists to provide medical detox coverage 7 days per week.
- A psychiatrist will be on-site 7 days per week to closely monitor patients in all levels of care.
- Medical provider onsite 7 days per week.
- Nurses are on-site 24 hours per day to address ongoing medical issues. There are multiple nursing stations on the property to ensure patients do not have to wait in line for their medications and assessments.
Residential Program
- The Residential Program generally lasts 14-21 days
- Patients will receive 4-5 individual or family sessions per week with their primary therapist
- Patients will begin completing assignments in the Life Skills Program
The Residential Program generally lasts 14-21 days with average length of stay being 15 days. During this time, patients will receive 4-5 individual or family sessions per week with their primary therapist and will have daily check-ins with their Life Skills Guide as well. Patients will begin completing a nightly Life Skills Planning worksheet and will begin each day by writing a daily schedule to follow that includes sleep goals, exercise goals, therapy goals, and nutrition goals. Additionally, they will begin completing other assignments in the Life Skills Program. Patients will see medical and psychiatric providers at least one time per week to continue adjusting medications or to address new or ongoing symptoms they may experience and will be evaluated by our nursing staff each day. They will have the option of eating nutritious meals in their patio area with their peers or in the privacy of their own bedrooms and will have nightly access to their personal electronic devices.
More Info on Residential ProgramResidential/Inpatient Treatment
- Offered at our Fort Myers and Plant City Locations
- Typical duration is 10-21 days
- Following the completion of detox, patients transition into residential/inpatient treatment
- In this level of care, you will continue to reside on our campus-style facility and are monitored 24 hours per day by nursing and behavioral health staff.
- Patients receive comprehensive, individualized treatment that includes multiple individual sessions with our professionally licensed staff, and are seen by medical and psychiatric staff a minimum of weekly.
- In residential treatment, your therapy is from 8 am to 4 pm. After that you become a guest and have a variety of services to choose from.
After 4:00 pm, some options are:- Go to our state-of-the-art recreation facility and athletic complex. One of the main reasons why our treatment is more effective than what other centers offer, is because of how we treat the patient when they are not in treatment. Having the recreation center is one of the most effective treatments we have. We have seen a much greater response to treatment because the patients are so comfortable during their stay.
- You will have access to personal electronic devices after, as long as it is used in your private room.
- Grass and sand volleyball courts are available
- You can sit by the pool and relax
- A variety of games and board games are available
- Work one-on-one with our personal trainers
- Participate in the boxing and fitness program
- Patients will be eligible to partake in multiple activities/amenities offered at the facility including chiropractic care, massage therapy, exercise facility, and yoga classes.
Day/Night (PHP) Program
- The Day/Night (PHP) program generally lasts 10-20 days
- Day/Night is the transitional phase of treatment where patients are beginning to move back into activities they would engage in at home
- They can reside in community housing or return to their home environments and commute to one of our outpatient locations for programming each day
- This allows them to receive freedoms slowly rather than all at once where they may become overwhelmed
The Day/Night (PHP) program generally lasts 10-20 days with the average length of stay being 14 days. Day/Night is the transitional phase of treatment where patients are beginning to move back into activities they would engage in at home and they experience increasing responsibilities. During this level of treatment, patients receive a reduced level of services commensurate with the stepped down level of care, however, continue to have access to some of the same amenities as described in our Residential Treatment Program. For instance, patients begin to attend group therapy 5-6 days per week instead of 7. They are able to reside in community housing or return to their home environments and commute to one of our outpatient locations for programming each day. They begin to self-administer their medications but are still able to consult with nursing staff during program hours and they begin to cook their own breakfasts and dinners again. Patients are able to participate in sober outings to surrounding areas and those residing in our community housing will have access to weekly shopping trips and receive increased access to personal electronic devices. This allows them to receive freedoms slowly rather than all at once where they may become overwhelmed. Patients who opted into the personal training program will be able to continue to exercise with their personal trainer on a daily basis and to engage in the boxing and fitness program (optional). Upon completion of this portion of the program, patients will be introduced to their outpatient therapist and primary care physician to provide a smooth transition into the next stage of their treatment and recovery.
More Info on Day/Night (PHP) ProgramDay-night/IOP levels of care [Transition from inpatient to outpatient environment with housing]
- Offered at our Fort Myers and Hyde Park locations
- At the point that your insurance and medical staff have decided you are ready to transfer out of residential treatment, you would then be sent to one of these locations.
- Typical duration is 14-30 days depending on your individual insurance company.
- This is a highly-structured day program that occurs 5-6 days per week and involves 5 hours of groups daily to further address addiction and transitioning back into society.
- Typically, patients that do detox and residential do that at our Plant City location, but we move you to Hyde Park or Fort Myers for this level of care
- Our professional staff is highly trained and used to working with other locations, where your file is seamlessly transferred and your care can continue
- Patients continue to receive multiple individual sessions per week and will see a psychiatrist weekly.
- Professional nursing staff is available during program hours to address medical issues, answer to a sick call, or for medication management.
- In this level of care, individuals can reside in their own homes or in the houses located on property.
- Lunch is provided daily but patients are responsible for preparing their own breakfast and dinner.
Intensive Outpatient and Recovery Program
- The Intensive Outpatient Program (IOP) can last anywhere from 30 to 90 days
- IOP entails participating in three hours of groups three days or nights per week
- Their Life Skills Guides will continue to check in with them daily for 90 days
- Allows patients to continue seeing their therapist for individual sessions
The Intensive Outpatient Program (IOP) can last anywhere from 30 to 90 days and the Recovery Program lasts a lifetime. IOP entails participating in three hours of groups three days or nights per week as well as individual sessions with a therapist and follow-up appointments with a psychiatrist and medical provider that you will have met during your earlier phases of treatment. During this phase of treatment, patients are either living at home or in a recovery residence and use their IOP programming to assist them in having increased levels of support during this early time in recovery. Patients can work full or part-time during this phase of treatment and resume many of their old responsibilities. Their Life Skills Guides will continue to check in with them daily for 90 days. The WhiteSands Recovery program (as detailed in our unique philosophies) allows patients to continue seeing their therapist for individual sessions as well as psychiatric and medical providers for a lifetime. This provides greater continuity of care and medical providers who know a patient’s history with trust already established.
More Info on IOP ProgramIntensive Outpatient Program with residence (IOP) further transitioning
- Offered at Fort Myers and Hyde Park locations as well as multiple offices throughout the state of Florida
- The typical duration of IOP is 30-90 days
- Following the completion of the day-night/IOP program, many patients choose to transition into an IOP program
- This program offers 3, 1 hour groups at 3 days a week as well as individual sessions and follow-ups with a psychiatrist. IOP is necessary for many individuals to maintain long-term sobriety and helps them ease back into coping with the stresses of daily life
- Recovery residences are available at our Fort Myers, Hyde Park, and St. Petersburg locations
- Patients in recovery residences are able to benefit from case management services including resume building, job interviewing, and life skills development
Staff Onsite 24/7
- Throughout detox, nurses monitor patients’ vitals and withdrawal symptoms 5 times per day and are seen by an addictionologist daily
- We have a minimum of 2 nurses working each detox station at all times and a behavioral health technician outside the detox rooms
- At the end of your 5-7 day detox, each patient will work with their therapist to agree on their individualized program
Within the Detox Program, each patient is seen by an addictionologist for a History and Physical Assessment and their individual therapist for a Chemical Dependency and Psychosocial Assessment within the first 24 hours. Throughout detox, nurses monitor patients’ vitals and withdrawal symptoms 5 times per day and are seen by an addictionologist daily.
At WhiteSands, we believe in staff always being available to patients; therefore, we have a minimum of 2 nurses working each detox station at all times and a behavioral health technician outside the detox rooms to provide any needed additional support. A patient only has to open their door and request assistance to receive help or to let a staff member know during their 30-minute safety checks. Each detox patio area, located directly outside the detox bedrooms, has comfortable seating and is stocked with food and drinks so that patients do not have to walk far in order to find food or beverages.
As the Detox Program progresses, patients in detox continue seeing their primary therapist multiple times to complete treatment planning, be introduced to the Life Skills Program, and to begin individual therapy sessions. They will additionally be introduced to their Life Skills guide who will be assisting them in developing a healthy and sustainable routine they can follow once discharged from treatment. At the end of your 5-7 day detox, each patient will work with their therapist to agree on their individualized program which will consist of including groups they will attend while also becoming familiar with their goals for therapy, physical health, and medication.
Customized Treatment Plans for Each Patient
- Patients will attend 5 groups per day, 7 days per week, and will receive a daily itinerary of groups, individual sessions, medical appointments, and personal training sessions
- This is all based on their individualized treatment program
- Our Trainers can assist patients in meeting health and exercise goals
During the Residential Program, patients will attend 5 groups per day, 7 days per week and will receive a daily itinerary of groups, individual sessions, medical appointments, and personal training sessions based on their individualized treatment program. Beginning in the Residential Program, patients will also have the opportunity to begin working with a personal trainer. WhiteSands employs full time personal trainers in our state-of-the-art recreation center. Our Trainers can assist patients in meeting health and exercise goals and introduce them to the benefits of boxing on physical and mental health. Our boxing is an entirely optional portion of the program, but has proven to be a popular one. Our boxing and fitness program consists of professional boxers and coaches who train patients in the physical and mental aspects of boxing, such as technique and strength and conditioning, using heavy and speed bags, training mitts, as well as fitness training.
What is a Typical Day in Residential Treatment
The theme at WhiteSands Treatment is that you are a patient from 8:30 AM - 4:30 PM, and from 4:30 PM to 11:00 PM, you become a guest. Once you become a guest, you are able to relax and enjoy the amenities. Guests can spend their free time enjoying whichever activities or amenities they wish, whether it’s exercising, partaking in activities and hobbies, or simply hanging out in your private room where you can watch TV and stay connected with friends and family.
Program Schedules
| 6:00 AM - 8:30 AM | Patients will wake up at 6am (or earlier) each day will be able to exercise in the gym, take medications, eat breakfast, and to complete their daily agenda. |
| 8:30 AM - 4:30 PM | Patients will attend 5 groups and see their therapist or medical providers per their individualized itineraries. Patients will have short breaks between groups as well as a lunch break and will have an hour of scheduled recreation to utilize the gym, the pool, or to relax in their bedrooms. |
| 4:30 PM - 10:30 PM | At 4:30 PM, patients become guests (as discussed in our innovative philosophies) and will be able to engage in a variety of recreational activities as well as recovery meetings. Their personal electronic devices will be waiting in their rooms when they finish groups, and they will be able to check in with family and unwind from a day of intense therapy. During this time patients will have dinner and will be able to learn to have fun while remaining sober. Please click below to see a list of activities available. |
| 10:30 PM (or earlier) | Patients will retire to their private bedrooms, complete their Life Skills Planning Worksheet, and go to sleep. |
After 4:30 PM, guests are welcome to:
- Use their cellphone/laptop or enjoy a flat screen tv in their private room
- Enjoy the gym
- Relax by the pool
- Take a walk
- Hang out in the lounge area
- Get a snack at the cafe
- Enjoy the rec. center and athletic complex
MAT Program
- MAT treatment is for individuals struggling with opiate addiction
- Allows patients to taper off opiates slowly while seeing a medical provider weekly
WhiteSands Treatment Center additionally offers a MAT (medication-assisted treatment) program for patients who have difficulty entering inpatient treatment for an extended period of time. MAT treatment is for individuals struggling with opiate addiction who have the ultimate goal of being off all addictive substances but who are unable to enter a detox program or detox from opiates within one to two weeks. Our MAT program allows patients to taper off opiates slowly while seeing a medical provider weekly. During MAT, patients are encouraged to participate in IOP or outpatient therapy as well and are able to receive the benefits of our WhiteSands Recovery Program.

Meet our Staff
WhiteSands Treatment has a team of highly-qualified addiction therapists, counselors, and specialists who are experts in the field of substance abuse treatment and recovery. Our team will work with patients daily, always putting the comfort and well-being of guests first. Achieving personal recovery goals is possible with the help of our staff.
Joseph Ducey, Chief Operating Officer, WhiteSands Treatment Center

Mr. Ducey currently serves as Chief Operating Officer of WhiteSands Treatment Centers and has held that position since before the opening of the facility.
As COO of WhiteSands, Mr. Ducey is responsible for the day-to-day operations of both the Fort Myers and Tampa treatment locations, which consist of over 180 beds combined. In addition to his day-to-day responsibilities at WhiteSands, Mr. Ducey was responsible for the implementation and expansion of WhiteSands locations at the direction of the owner and CEO, Garry Jonas. The vision was to build a treatment center that put both patient comfort and individualized care as the center point of our program, employing the best in the business to deliver second-to-none treatment.
Before joining WhiteSands, Mr. Ducey held a variety of management positions within Acquinity Interactive and its subsidiary companies, where his responsibilities primarily focused on the day-to-day operations of the call center management team, product development, and implementation and analysis. Prior to joining Acquinity, Mr. Ducey served as Executive Vice President of CIT Group in Livingston, New Jersey, where he was responsible for all trading and securitization activities. He holds a degree in Business Administration from Rutgers University in New Jersey.
Mr. Ducey currently resides in Fort Myers Florida.
Lyndsay Henry, Clinical Director, WhiteSands Treatment Center, Ft Myers

Lyndsay Henry, Ph.D. currently serves as Vice President of Clinical Services for all WhiteSands locations and has held that position since shortly after the opening of WhiteSands in 2014. She divides her time between both the Fort Myers and Tampa locations.
Within these roles, Dr. Henry oversees the clinical operations for all locations. She is responsible for hiring and training all clinical staff in Fort Myers and Tampa as well as creating and implementing the program schedules and aiding in ensuring that patients receive the best treatment possible. Dr. Henry is a licensed Clinical Psychologist in the state of Florida; she received her undergraduate degree in Psychology and Sociology at Vanderbilt University in Nashville, TN. She has her master’s and doctorate degrees in Psychology from Nova Southeastern University in Fort Lauderdale, Florida. She has worked extensively with children, adolescents, and those struggling with addiction.
Dr. S. Mann, M.D., Chief Medical Officer, WhiteSands Treatment Center

Dr. Mann currently serves as the Chief Medical Officer and Medical Director of the WhiteSands Treatment Centers and he has held these positions since July 2017. In addition to medical department administrative duties, Dr. Mann is responsible for the medical needs and detoxification of patients at WhiteSands Treatment, Tampa.
Before joining WhiteSands, Dr. Mann has worked in addiction treatment facilities throughout Florida. He has served as an Adjunct Clinical Postdoctoral Associate in the Addiction Medicine Division at the University of Florida, where he enjoyed teaching medical students and medical school graduates during their residency training. He has also practiced Addiction Medicine in the private sector and served as both Medical Director and Associate Medical Director at other substance abuse treatment centers. He currently enjoys both clinical duties and oversight roles as Medical Director of WhiteSands Treatment Centers. Dr. Mann appreciates the teamwork at WhiteSands and how this helps patients resume a happy, fulfilling life.
Dr. Mann graduated with honors from Indiana University where he earned both his Medical Degree and a degree in chemistry. He completed his internship at the University of Miami-Jackson Memorial Hospital before completing his residency in Internal Medicine at Mount Sinai Medical Center in Miami Beach, FL. He later studied Addiction Counseling in Denver, Colorado and he completed an Addiction Medicine Fellowship in the Psychiatry Department at the University of Florida. Dr. Mann is Board-Certified in his field.
Karen Lopez, M.S., Director of Quality Assurance, WhiteSands Treatment Center

Karen Lopez currently serves as the Director of Quality Assurance for WhiteSands Treatment. Ms. Lopez graduated with a Master’s Degree in Healthcare Administration from the University of Maryland and has been working in the healthcare sector for over 10 years. She has been working with WhiteSands for the last three years where her role includes coordinating the admission and discharge processes, as well as maintaining high standards of quality assurance. As someone who has witnessed family and friends struggle with drug and alcohol addiction, she states, “I wanted to be part of a team that genuinely cares and works to help those in their most desperate times. I am proud to be part of a team that understands that addiction affects all walks of life, and prides itself on providing an outstanding, comprehensive approach to treatment.”
Valerie Deacy, R.N., Director of Nursing, WhiteSands Treatment Center

Valerie Deacy currently serves as the Director of Nursing for WhiteSands Treatment Center, Tampa. Mrs. Deacy graduated from Kingsborough College with an AAS degree in Nursing.
She has been part of the healthcare industry for the last 15 years, specializing in working with patients who struggle with all forms of addiction and substance abuse. Valerie has been the Director of Nursing for WhiteSands since 2017. “Seeing the transformation in patients while they are in treatment is the most rewarding part of my job".
All Things Non-Medical/Clinical - Amenities, Activities, Accommodations and Food
At WhiteSands, we believe that patients deserve to be in comfortable accommodations and be treated with respect and dignity throughout their stay. We put a great deal of emphasis on this, because we have recognized that a comfortable guest makes for a successful patient (one of our innovative philosophies discussed in other sections of our program description). Patients are treated as guests from 4:30 PM, which is the conclusion of a rigorous day of groups and individual sessions, until 8:30 AM the next morning. We have seen evidence that treatment absorbs better when this occurs; thus, we believe that this will lead to increased rates of sobriety following completion of treatment. Here is a description of our amenities:
The main issue that individuals who sought treatment ran into was that these centers made treatment as if it was a torture test. They wanted to see if the patient could last the 30-60 days required for treatment with no creature comforts at all. To us, the average facility has the mentality of, “we understand that you are giving up your substance of choice and preparing to go through that is hard enough, but now let’s take away your cell phone, your privacy, restrict your television viewing time; let’s take away virtually all of your ‘creature comforts’ including no contact with your loved ones and no access to food that you enjoy”. This isn’t just a substance abuse rehab center anymore; it is a torture test of all habits and no one would thrive under these conditions. Naturally, this creates agitation and patients begin to do whatever it takes to simply get through treatment and get out.
Understanding what the treatment industry lacked and knowing how we wanted to make it better, allowed us to cultivate a simple philosophy: let’s make guests as comfortable as possible by placing a large focus on the wellbeing of our patients.
"Let’s make guests as comfortable as possible and by doing so, get better results with treatment".
Rooms/Property
WhiteSands is housed on a spacious, 10-acre property that is set up in a campus style environment. We offer private rooms with queen-sized beds, full bathrooms, and flat screen satellite televisions to allow for a private and tranquil place to unwind each evening. This allows patients to learn to “sleep right,” which is an important component of our Life Skills Program. Patients are able to complete homework assignments and reading, check-in with family members, and decompress without being distracted by others. This can lead to increased focus and decreased anxiety.


Food
At WhiteSands, we prepare healthy and nutritious meals each day on-site, and we emphasize the need for a healthy diet through the “eat right” portion of our Life Skills Program. We have a dedicated kitchen staff that is able to meet dietary restrictions and provide multiple food options. This allows patients to begin to return to a state of physical health, when in their addiction they were often overeating or undereating.


Spa
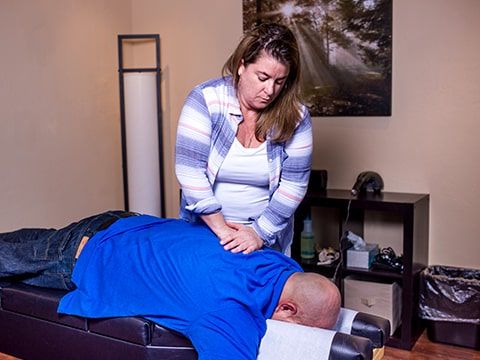
At WhiteSands, we recognize that many patients were self-medicating anxiety, stress, and physical pain with their addictions. Due to this we provide chiropractic care, massage therapy, and biofeedback. For many patients, their chronic pain and stress is due to poor self-care, and we want to assist them in recognizing that they can engage in healthy activities daily that reduce the need for self-medication. The spa services and relaxation techniques assist in the “sleep right” portion of our Life Skills Program.


Physical Health
At WhiteSands, we have a state-of-the-art recreation center to allow patients to exercise or engage in personal training daily. We have a large boxing ring, a cardio section, a yoga area, and a weights section to suit everyone’s needs. Personal training is beneficial for those who have never exercised before or who struggle with poor self-esteem and shyness that prevent them from entering a crowded gym. Physical health is an important component of our Life Skills Program.


















click arrows to see more testimonials
Boxing and Fitness
As a component of the physical fitness program, WhiteSands offers a one-of-a-kind specialized boxing program where patients are able to be trained by professional fighters and coaches using professional grade boxing equipment and heavy / speed bags and boxing mitts. Because this can be done within a personal training session, we can meet the needs of the typically sedentary individual and the needs of former professional athletes. Patients and alumni are able to witness professional boxers both spar for upcoming matches and attend the actual fights. Being successful in boxing, much like being successful in sobriety, requires day to day effort, determination, and focus. Boxing has many therapeutic benefits including allowing for unparalleled releases of frustration and anxiety, requiring complete focus and increasing concentration, increasing self-esteem and the belief that you can be powerful and protect yourself, and serving to exhaust the body and lead to a better night’s sleep. Boxing assists many people in slowing their thought processes and reacting in less impulsive manners. Many of our alumni have continued a boxing training regimen in their hometowns and have discussed how it aids them in maintaining their sobriety.


Electronics
At WhiteSands, we recognize that cutting patients off from all social and family contacts while in treatment, can be detrimental to lasting recovery. If patients are fully isolated while in treatment, they are often bombarded with voicemails, text messages, emails, and social media when they return home. This can lead to rapid relapses. Due to this, we provide nightly access to personal electronics for patients fully participating in all groups and individual sessions. This allows them to check messages daily, have lengthy conversations with family members, and be exposed to some “real-world” stressors while in a supportive treatment environment with staff nearby. Allowing patients to experience some inevitable conflicts with friends or family while having easy access to staff members and therapy, allows them to deal with this trigger within a supportive environment.



Activities
During the guest hours (4:30 PM - 10:30 PM), we offer a variety of activities on our large and resort-like property. When entering treatment, many individuals struggle with the belief that they will never be able to engage in social activities or have fun while sober. We challenge this nightly and work to have each individual identify sober activities and hobbies they can continue when they return home. We offer both small group and larger group activities that include karaoke, board game tournaments, corn hole games, basketball, volleyball, ping pong, escape rooms, and movie nights. Patients have access to pools to exercise or socialize in as well as a large entertainment complex with large screen televisions. As patients transition through levels of care, they begin to be exposed to off campus sober activities as well with trips to the bowling alley or beach. This allows for activities for all ages and interests.


10-Acre Campus - Room to Breathe
Our main goal was to provide ample space and room to breathe for all patients. If an individual is going to stay 30-60 days and be in a good frame of mind, having enough space to roam around is a very important element so that patients don’t feel cramped or crowded.
When patients are not attending treatment or therapy, they are welcome to enjoy the wide range of amenities that are offered at the facility, much of which would not be accessible without our significant investment in a 10-acre campus.
Private Rooms - Peace of Mind
When we invested in our Tampa residential campus, one of the things that attracted us to the property was the number of rooms it offered. This allowed us to provide private rooms to each guest. The newly renovated private rooms feature a flat-screen TV, queen-sized bed, and a private bathroom which allows patients the privacy to be comfortable and relaxed before and after treatment hours.
Everyone wants and deserves privacy which is why we offer this private room feature. Not many individuals can last very long sharing a room with a random person. Our approach is different; we aren’t trying to strip you of all the comforts of home but rather, believe that having these luxuries, such as a private room and all that it has to offer, truly aids in the recovery process. We understand that you have to take care of life while you are here and our policies are conducive to that.
We aim to make patients as comfortable as possible because when individuals feel comfortable in their environment, they are much more likely to digest therapy.
Please call for more information.


Cell Phones/Devices Allowed - Staying in Touch
We decided on a lenient cell phone/electronics policy that allows guests to use their cell phones and electronic devices from 4:30 PM to 10:30 PM. Allowing guests to stay connected with friends and family provides peace of mind, lowers anxiety, and makes for a more comfortable stay.
To protect the privacy of fellow patients, cellphone and laptop use are prohibited in common areas. We understand that being admitted to treatment is an overwhelming adjustment in itself, and taking away personal electronics can make a guest feel disconnected and isolated. We went the extra mile to ensure that our guests have access to their personal electronic devices before and after treatment hours, putting us a step above other treatment centers.
We understand that you must be able to interact with the outside world while in treatment. Having access to therapists who can help you handle some of the personal issues that come with communication from the outside world during your 30 or 60-day stay is very beneficial and can help you better grasp and control emotions during this time of change.


Brand New Recreation Center - Pass the Time
Our facility features a newly-constructed recreation center where guests can enjoy a range of activities in their free time. The center features a snack bar, refreshment stand, and lounge area where individuals can kick back and relax. The recreation center is more than just a place to catch up with fellow guests and share some laughs; it brings a sense of community, builds friendships, and allows for the development of healthy hobbies and habits. Some of the activities that guests can enjoy in the rec. center are:
- Ping pong
- Watching major sporting events and movies on a large, theatre-sized screen
- Enjoy a snack/refreshment
- Playing cards and board games
- Socialize and mingle with other guests
- Yoga Classes
- Listen to music
- Relax on the patio at night
- Enjoying a BBQ



Activities to Enjoy - Have Some Fun
Our facility offers patients the chance to enjoy a range of recreational activities when they are not in treatment or therapy. From walking paths that lead to tranquil fountains and gazebos, to boxing, and yoga; WhiteSands has countless options when it comes to enjoying your free time.
Some of the activities that can be enjoyed when guests are not in treatment are:
- Enjoy the pool
- Volleyball
- Basketball
- Yoga
- Watch a movie on the big screen
- Ping-Pong
- Enjoy walking paths
- Relax in the gazebo
- Designated smoking areas
- Arts and crafts
- Badminton
- Cornhole
Keeping busy through exercise and activity is a great way to get fit while creating new hobbies and habits that can help you lead a healthy and happy life, post-treatment.
Newly Constructed Athletic Complex - More to do
Our facility features a newly-constructed state-of-the-art, 15,000 square foot athletic complex featuring a range of exercise equipment and activities. This includes ellipticals, treadmills, and stationary bikes, among others, as well as a full-sized boxing ring. Boxing is a great means of therapy and is an effective way to manage stress, anxiety, and the different emotions that come with the treatment process. There is something for everyone at our new athletic complex, whether you are looking for a moderate workout or wanting to hone in on self-defense tactics; we offer a wide selection of activities for those of all athletic abilities to take part in.
This athletic complex is something that no other treatment center provides at this level. Please see the presentation for details on the fitness and boxing programs.


Fitness Programs and Personal Training - Get in Shape (Optional)
Our team of specialists will work with patients to construct a fitness and nutrition program that is tailored to their unique needs. As the patient gradually overcomes and learns to manage their addiction during treatment, personalized fitness programs can be implemented as this will help them create new, healthy habits. We feel strongly that fitness and nutrition are a big part of combating temptation and cravings.
What patients may not realize is that a balanced, nutrition-rich diet can help them better manage withdrawal symptoms such as lack of concentration, anxiety, cravings, and insomnia. We have also seen that exercise, coupled with good nutrition, promotes better sleep. Our theme here at WhiteSands is that eating well, sleeping well, and exercising regularly are important components in achieving long-lasting recovery.
For those who are not very athletic or have not been trained before, there is no need to worry. Our staff is very sensitive to this reality and we have programs for all different fitness levels and abilities. We have programs offered at certain times throughout the day that are allocated to beginners, intermediate, and advanced; our programs are designed for all.


















click arrows to see more testimonials
Boxing Program - Blow off Steam (Optional, Tampa Only)
The owner of WhiteSands Treatment is a boxing enthusiast and a hobby of his is training and managing professional boxers. His professional boxers and coaches use the WhiteSands gym during the day while patients are in treatment. From 6 am to 7 am and from 4 pm to 8 pm, his team of trainers and fighters focus solely on training and helping the patients.
All our patients who have tried the boxing program have experienced significant therapeutic benefits. This is truly a program that we believe works for everyone. For those of you who think this isn’t for you, we have a long list of clients who felt this same way until they tried it. Men, women, young, old, and the physically challenged all get significant benefits from the mental, emotional, and physical release that boxing training provides. The owner only asks that everyone try it just once. Please see the video testimonials.
Some of the benefits of our boxing program are:
- Amazing therapeutic results
- Better sleep patterns
- Feeling more alert
- Lessened anxiety
- More relaxed
Boxing has proven to be beneficial in the recovery process and many guests who partake in this program have continued boxing post-treatment.
Life Skills Program
- Each patient gets a life skills guide who works with them daily to help this become a healthy habit long-term
- The overall philosophy of the Life Skills Program is that we want to assist each patient in not only developing the skills to maintain long-term sobriety, but we also want them to live their most successful, happy, and balanced life possible
- We assign each patient a Life Skills guide to assist in improving eating and sleeping habits and to help create a daily routine, schedule, organization skills, and planning that helps to live a balanced, healthy, and happy lifestyle
- Our Life Skills Guides conduct check-ins throughout the patients involvement in the WhiteSands Recovery and Wellness program
- Each patient will be assigned a personal trainer and nutritionist throughout their treatment stay (optional)
At WhiteSands we recognized how many of our patients thrive in treatment and then struggle to create a routine and healthy lifestyle once they return home, which ultimately leads to relapse. We, therefore, decided to create a Life Skills Program that would assist patients in learning to sleep right, eat right, and live right on a daily basis. The overall philosophy of the Life Skills Program is that we want to assist each patient in not only developing the skills to maintain long-term sobriety, but we also want them to live their most successful, happy, and balanced life possible. For many patients their addictions led to a chaotic and disorganized lifestyle where anxiety and impulsiveness were significant issues that led to substance use. When living in chaos, people tend to skip meals, eat unhealthy foods, have unhealthy sleep patterns, run late, and not meet family and work goals. This can lead to poor focus, irritability, mood swings, increased depression, weakened immunity, and weight gain.
Through our Life Skills program, we assign each patient a Life Skills guide to assist in improving eating and sleeping habits and in creating a daily routine and schedule that helps to live a balanced, healthy, and happy lifestyle. This leads to greater success in personal and professional areas and decreased relapse rates. Our Life Skills program is implemented through weekly sessions with a therapist and daily check-ins with a Life Skills Guide. This leads to patients being able to “plan their work” and “work their plan”.
Our Life Skills program works to meet the needs of all patients, as it is conducted on a one-on-one level. We work to help patients be able to identify the progress and areas of weakness they face each day, identify and complete healthy goals, and find balance in all areas of their life. We have each patient complete a detailed relapse prevention/continuing care plan that addresses not only addiction to substances but all compulsive behaviors. Life Skills Guides conduct check-ins and remain in contact with and accessible to patients for as long as the patients are actively involved in the WhiteSands Recovery and Wellness program, which may include continued participation in outpatient therapy, seeking medical or psychiatric services from one of our providers, or maintaining pharmacy services through our affiliated pharmacy.
This program has been extremely popular with our patients. Some patients were resistant; however, once they saw that they could create their own program with their life skills guide, they were extremely pleased with the results. We work with patients to adapt the life skills program to their individualized needs to increase the likelihood they will implement it not only in treatment but also once they return to their home environment.
Relapse Prevention
- WhiteSands created a Recovery and Wellness Program to help address concerns that come with the transition between leaving inpatient treatment and entering the next phase in the recovery process
- Patients in our outpatient program are also able to continue seeing the same doctors and psychiatric providers once they return home
- We believe that taking this approach will lead to increased long-term sobriety rates and will allow us to monitor its impact on our patients and their road to recovery
At WhiteSands, we recognize that nationwide relapse rates are abysmal and something that we want to work to change. The standard relapse prevention groups and work has not been successful for the majority of individuals struggling with addiction. We have made many changes to our program experience in addressing the prevention of relapse.
As part of our program, we have patients complete relapse prevention plans related to substance addiction while also having them identify areas where they might fall into other addictive patterns once they return home. Many individuals with addictive personalities achieve initial sobriety from drugs and alcohol but begin exercising compulsively, restricting food, overeating, working 80 hours per week, or engaging in compulsive sexual behaviors. Engaging in any of these behaviors often leads to relapse on substances while also causing issues in their personal lives, just like their substance use issues did.
We also recognize that many patients successfully complete inpatient treatment but then do not complete recommended intensive outpatient treatment, do not attend medical follow-up appointments, and do not remain medication compliant. All of these behaviors often lead to relapse, and patients are additionally losing the structure, accountability, and medical care that assisted them in succeeding in inpatient care. When discussing reasons why alumni did not engage in follow-up care, we learned that there were common reasons. These included not wanting to tell their story to a new doctor or therapist and difficulty finding doctors to refill their medications. Therefore, WhiteSands created a Recovery and Wellness Program to help address these concerns so they are not a barrier to sobriety. Patients are introduced to their outpatient therapist by their inpatient therapist and relevant information and history is discussed during the last week of inpatient. With this approach, the patient knows who they will be meeting with the following week. Patients in our outpatient program are also able to continue seeing the same doctors and psychiatric providers once they return home, so that their providers know their history and which medications have achieved the greatest effect. Patients will also have access to a 24-hour hotline and multiple virtual alumni and check-in meetings that occur daily for support with their sobriety.
Patients in our inpatient settings also receive 4-5 individual or family sessions per week as well as the Life Skills Program discussed in other descriptions of our services. This allows for greater processing of the issues that contributed to their addiction and increased family involvement. We recognize that if a patient returns home to the same environment without engaging in therapy with their loved ones, they will often relapse. The Life Skills Guide additionally provides for greater accountability throughout lifelong sobriety. We believe that taking this approach will lead to increased long-term sobriety rates and will allow us the ability to monitor its impact on our patients and their road to recovery.
How Does WhiteSands Compare to Other Treatment Centers
Clinically and medically we consistently provide more than industry standards require. Our clinical and medical staff recognize that we need to provide more in-depth and individualized treatment in order to meet the critical needs of our patients. As a result of our commitment to providing the highest quality of care, we have a higher percentage of patients with sustained recovery. Please see the list of highlights below:
- Individual or family therapy five times per week, where other agencies offer one hour per week.
- Truly individualized treatment that results in smaller groups and a high staff-to-patient ratio despite the narrowing of profits.
- Full-time skilled and highly-credentialed staff dedicated to all stages of treatment/recovery, resulting in better continuity of care and a total focus on patient outcomes.
- Truly unique Life Skills Program, which increases success when patients leave our treatment facilities, as well as provides continued daily support following discharge.
All of the above comes with either significant investment or greater operating costs. We go above and beyond because of our commitment to our patients and their outcomes.
With regards to patient experience while not in treatment, the strength of our amenities and the overall quality of life at WhiteSands are of significant importance to our leadership team and staff. We strongly believe that a patient’s comfort level during their stay has a strong correlation to their success in treatment. We have witnessed that their ability to focus and absorb information is correlated with them feeling calm and comfortable. Please see the list of highlights below:
- Large private rooms with satellite television and private bathrooms.
- Use of electronic devices in room from 4:30 PM - 10:30 PM nightly to allow contact with loved ones and management of life outside of treatment. This policy allows patients to receive the value of limited distractions while in treatment, while also allowing for continued connection with the outside world. Importantly, if patients are triggered by calls or messages they receive, they are doing so while in a highly-supportive environment rather than facing this for the first time at home alone.
- State-of-the-art athletic complex and boxing gym.
- Personal training with professional athletes and coaches.
- Large campus with pool, basketball, and volleyball courts.
- Strict COVID testing and safety protocols.
Once again, all of the above demonstrates our investment and dedication to your recovery journey. These are just some of the ways we continue to raise industry standards.
Overall, there is no other treatment center for private insurance that provides all of the above.
Click here to see an 18 point comparison between WhiteSands and the average treatment center
Accommodations
When you're considering going to treatment, you cannot underestimate the living accommodations when you are staying there for 30-60 days. We put a lot of effort into making sure people are comfortable on our campus and in our rooms so they can focus on their recovery. Everyone wants and deserves privacy. Not many individuals can last very long sharing a room with a random person. Treatment centers shouldn’t be trying to strip all the comforts of home. A private room and all that it has to offer can aid in the recovery process, which is what we offer.
Industry Standard
Most facilities operate out of cramped office buildings or small houses with not much room to roam. You will also have 2 to 3 people per room with small twin beds, often no TV, and a bathroom that is shared.
WS PREMIUM
With WS premium you will get your own large private bedroom with a private bathroom and a TV.
10-Acre Campus
If an individual is going to stay 30-60 days and be in a good frame of mind, having enough space to roam is a very important element so that patients don’t feel cramped or crowded. At WhiteSands we have enough room to provide a full volleyball court, a large basketball court, and a resort-style pool for the enjoyment of our guests. Most facilities lack any real outdoor space, resulting in a cramped, congested feeling for the entirety of your stay.
Industry Standard
Small, cramped locations with very little space to enjoy.
WS PREMIUM
10-acre campus with a variety of amenities including a pool, volleyball, basketball, a recreation center, a state-of-the-art athletic complex, as well as plenty of room to stretch out and relax.
Cell Phones/Electronics Allowed
Being admitted to treatment is an overwhelming adjustment in itself, and taking away personal electronics can make a guest feel disconnected and isolated. You must be able to interact with the outside world while in treatment. Having access to therapists who can help you handle some of the personal issues that come with communication from the outside world is very beneficial and can help you better grasp and control emotions during this time of change. Managing this is time-consuming so most facilities just decide to deny access to all electronics during the entire treatment program.
Industry Standard
No real access to electronics. You might be allowed a supervised call on occasion.
WS PREMIUM
Access to cell phones and electronic devices including tablets and laptops from 4:30 PM -10:30 PM after detox.
Recreation Center
A recreation center is more than just a place to catch up with fellow guests and share some laughs; it brings a sense of community, builds friendships, and allows for the development of healthy hobbies and habits. A recreation center makes your stay more enjoyable. Many treatment programs do not offer a recreation center.
Industry Standard
Unable to provide a recreation center. They might have some board games or books you can use.
WS PREMIUM
Our center features a snack bar, refreshment stand, and lounge area where individuals can kick back and relax. Guests can also play-ping pong, cards, or board games, watch a major sporting event on large, theater-sized screens, take yoga classes, or simply relax and listen to some music.
Athletic Complex
An athletic complex features a wide range of exercise equipment and activities. This includes free weights, ellipticals, treadmills, and stationary bikes, among others. Exercise is a great means of therapy and is an effective way to manage stress, anxiety, and the different emotions that come with the treatment process. Most facilities will not have any gym, let alone an entire athletic complex. Some may have a small room somewhere on-site with some old equipment.
Industry Standard
Some facilities will have a few pieces of old exercise equipment, such as a treadmill and some weights in a small room on-site.
WS PREMIUM
Access to a 15,000 sq. ft. state-of-the-art athletic facility with exercise equipment including free weights, ellipticals, treadmills, and stationary bikes as well as a professional boxing ring and training equipment.
Professional Boxing Training Program by Professional Coaching Staff
Boxing has proven to be beneficial in the recovery process. Many of our patients who have participated in our boxing and fitness programs continue their training after they have completed our programs and returned home. Men, women, young, old, and the physically challenged all get significant benefits from the mental, emotional, and physical release that boxing training provides. Boxing training has been linked to better sleep patterns, lessened anxiety, as well as feeling more alert. WhiteSands is the only rehab to provide professional boxers and coaches to work with patients and is an optional feature of our program.
Industry Standard
No access to any type of boxing program.
WS PREMIUM
Access to individual classes with professional boxers and coaches. When not in boxing class, guests have access to both types of bags (speed and heavy).
Personal Training/Nutrition Plan
As the patient gradually overcomes and learns to manage their addiction during treatment, personalized fitness programs can be implemented as this will help them create new, healthy habits. These healthy habits also include what you eat. Our nutritionists will customize a meal plan to meet your individual needs. Considering most facilities do not provide much in the way of gym equipment, they are not likely to provide any personal training or customized nutrition plans.
Industry Standard
No personal training or customized nutrition plan.
WS PREMIUM
Ability to schedule personal training sessions. During these sessions, the personal trainer will build a customized plan catered to the fitness needs of each individual. They will also work with your nutritionist which works with each patient in building a nutrition plan.
Dining Services
What patients may not realize is that a balanced, nutrition-rich diet can help them better manage withdrawal symptoms such as lack of concentration, anxiety, cravings, and insomnia. At WhiteSands, we provide home-cooked, quality food including an 18-item salad bar.
Industry Standard
Catered food.
WS PREMIUM
Delicious quality food, home-cooked and prepared on-site, including an 18-item salad bar. Gourmet espresso coffee and weekly steak BBQ.
One-on-One Therapy Sessions
Greater individual attention yields greater outcomes as the therapy is more individualized and the therapists have more extensive training. Relying on group sessions as the majority of the program does not allow sufficient time to address patient-specific issues but is often done to counter the expense of individualized care. The industry standards generally call for one individual session per week, which does not provide the time patients require for treatment to be effective and in allowing them the opportunity to really understand their recovery and how to effectively handle life stressors in sobriety.
Industry Standard
A single, one-on-one session per week.
WS PREMIUM
Patients will receive four individual sessions with their primary therapist per week.
Individualized Programs
Most treatment centers use a generic, one-size-fits-all approach to recovery that does not offer a personalized or individualized treatment plan. When the underlying issues are not addressed, many patients relapse because they have not learned coping skills for specific triggers which may lead them to using substances again.
Industry Standard
A generic, one-size-fits-all approach to recovery.
WS PREMIUM
Fully customizable treatment plan.
Relapse Prevention
We address relapse prevention throughout all levels of treatment. Our relapse prevention education begins during detox and continues throughout our outpatient program. While patients are in the inpatient phase of treatment, they are insulated from many triggers and have staff available to process cravings with them 24 hours per day. Both in the inpatient and outpatient phases of treatment, patients have Life Skills Guides available to check in with them daily, both to continue their life skills training and to ensure they are not at risk of relapse when at home.
Industry Standard
Set up patients with a referral to an outpatient program.
WS PREMIUM
Your life skills guide will be working with you to prepare for your aftercare while you are onsite with us. That guide will then be working with you over the first 6 months of your recovery to ensure you have the support you need. You will also be able to attend any one of our 16 outpatient locations for long-term OP therapy. Access to our network of psychiatrists and primary care physicians for continued healthcare. Our Alumni team and the corresponding network of alumni will be there to support patients on their journey to life-long sobriety.
Life Skills Program
A Life Skills Program provides patients with the long-term support they need when they transition back home or into a continuing care program. Life Skills Guides begin their work with patients during the detox phase and then transition through all levels of care with them. This provides them with greater continuity of care and is a crucial component of maintaining sobriety during the first 6 months. Leaving patients to fend for themselves when they go home, after having continued support for up to 45 days of inpatient care, is a big change that many patients are not ready for, which often leads to early relapse.
Industry Standard
No life skills program or guide provided.
WS PREMIUM
Life Skills Guides begin their work with patients during the detox phase and then transition through all levels of care with them. This provides them with greater continuity of care and is a crucial component of maintaining sobriety during the first 6 months. Leaving patients to fend for themselves when they go home, after having continued support for up to 45 days of inpatient care, is a big change that many patients are not ready for, oftentimes leading to early relapse.
Trauma Therapy
Many patients struggle with a significant traumatic past and require trauma therapy to fully recover. Leaving past traumas such as physical or mental abuse untreated, while expecting patients not to self-medicate, is only setting them up for failure. If patients are to fully recover, then the issues leading to chemical dependency must at the very least begin to be treated while the patient is in inpatient, and ideally continued throughout the relapse prevention portion of the program.
Industry Standard
You will find that most treatment centers do not provide trauma therapy for several reasons: First and foremost, trauma therapy is a specialization that requires advanced training which is expensive, and secondly, trauma work requires one-on-one work over an extended period of time. The standard for most treatment centers is to not incorporate trauma therapy in their overall treatment programming, which can undermine the recovery process and impact sobriety.
WS PREMIUM
WhiteSands premium program incorporates trauma therapy to those patients that benefit from it, beginning in inpatient care and continuing in outpatient care for as long as a patient is willing to participate. Trauma, as it pertains to drug and alcohol addiction, must be addressed in those patients suffering in order to give them the best chance at sustaining long-term sobriety. Otherwise, we are detoxing patients without addressing the underlying issues that have led patients to self-medicate.
Family Therapy
Family therapy is an essential part of treatment as patients will have difficulty maintaining sobriety if they return to the same stressful environment they were in prior to entering treatment. Addiction affects all members of a family and support system, and the family needs support and tools to assist the patient in maintaining sobriety and to begin to restore damaged and neglected relationships.
Industry Standard
Standard treatment centers generally do not provide family therapy while a patient is in inpatient care. Family therapy takes time and resources on the part of the treatment center and requires exceptional staff that are able to get patients' families to accept that there are family dynamics which contribute to the addictive patterns.
WS PREMIUM
Family therapy is an important part of WhiteSands’ treatment program. Not only do we provide family therapy as a group endeavor, but we also treat other members of the family unit that may be suffering from their own issues. Any member of a patient’s family may struggle with their own issues separate from drug and alcohol dependence. By treating the whole family, we are ensuring that patients are returning to a positive healthy environment, with the support of family members that can relate through their own experience.
Full-Time DR’s on-Site
It is important to have full-time addictionologists, psychiatrists, and medical providers on-site rather than having visiting physicians that work at a number of programs. This is an important step in ensuring that patients have focus and continuity of care of medical providers as we work to stabilize their health.
Industry Standard
Most facilities have visiting physicians who do not keep office hours on site. They will only come in for a set amount of time each day, and may not be there every day.
WS PREMIUM
We provide on-site addictionologists, psychiatrists, and other medical providers who have full-time office hours on the property.
Outpatient Transition
Many patients thrive in the structure of an inpatient treatment environment but quickly relapse when they return back to their home and work environment. We provide a step-down approach through all levels of care so freedom is gained back gradually. Support and the ability for patients to participate in continued outpatient therapy is an important part of the ongoing recovery process. We have 16 locations throughout the state of Florida; many treatment center’s need to refer patients to other centers in order to complete each step-down.
Industry Standard
Most facilities need to refer you to another treatment center for your outpatient/aftercare.
WS PREMIUM
You are able to receive all of our outpatient and aftercare services at one of our 16 strategically placed locations. Because of our vast outpatient offering, many patients will have access to our outpatient services in or near their hometown.
Biofeedback
Biofeedback is a specialized therapy that is of great therapeutic value in reducing anxiety and depression, and can help enhance healthy sleep patterns and promote an overall sense of relaxation.
Industry Standard
Most facilities do not provide Biofeedback.
WS PREMIUM
Patients have access to Biofeedback up to 5 times per week.
Spa Services
Spa services allow patients to indulge in much-deserved self-care which is an essential part of the overall recovery journey. By offering a range of spa services to enjoy that are designed for the patient's well-being, they can relax both body and mind in a serene and calming environment.
Industry Standard
Most treatment facilities do not offer any type of spa services for patients.
WS PREMIUM
With WS Premium, patients have access to a selection of spa services such as massage therapy, chiropractic services, and haircuts.
Which WhiteSands Facility is Right for Me?

Fort Myers Features:
- Inpatient Detox (Medically Assisted Detox)
- Residential/Intensive Inpatient Treatment
- Day-night Treatment [Transition from inpatient to outpatient environment with housing]
- Intensive Outpatient Treatment with residence (IOP) with residence [Transition from day/night to outpatient treatment]
- Resort-like atmosphere with gazebos, streams, and walking paths to avoid the institution feel.
- Maintains a small population of 20-30 patients
- Bedrooms include full-sized beds in private rooms.
- Cell phone and laptop access are available nightly following completion of detox.
- Housing is villa style with 4 bedrooms per house and a living room in each house.
- Our residential services include updated, private rooms providing the privacy patients need for a successful recovery
- 2 pools are available for patients to utilize after group hours.
- Basketball hoop, corn hole, and other recreational activities available.
- Gym open daily to promote a healthy lifestyle.
- Off-site outings offered to aid patients in learning to have fun in sobriety. Outings include trips to the bowling alley, the park, and the beach.
- Barbeque grills are located throughout the property.
- High quality catered foods from local restaurants.
- Patients within day/night levels of care prepare and cook their own food.
- Chiropractic care is offered as an amenity to assist patients struggling with chronic pain.
- Yoga classes are offered multiple times weekly. These include a blend of stretching and active classes.
- Spa Services available.

Plant City Features:
- Inpatient Detox (Medically Assisted Detox)
- Residential/Intensive Inpatient Treatment
- Day-Night Treatment [Transition from inpatient to outpatient environment with housing]
- Intensive Outpatient Treatment with residence (IOP) with residence [Transition from day/night to outpatient treatment]
- Bedrooms include queen-sized beds and the option of private rooms. Televisions are available in each room, as well as a private bathroom and shower.
- Cell phone and laptop access are available nightly following the completion of detox.
- Large pool is available for patients to utilize following the completion of detox.
- Resort-like atmosphere with gazebos and tiki huts to avoid the institution feel.
- Basketball court, grass volleyball court, and sand volleyball court available on property.
- 15,000 Sq ft. professional grade athletic complex open daily to promote a healthy lifestyle.
- Newly-constructed state-of-the-art recreation facility.
- Professional Boxing training program by professional coaching staff.
- Outdoor barbeque cookouts with freshly grilled food to order.
- Quality food, home cooked on site. 18 item salad bar.

Hyde Park Features:
- Day-Night Treatment [Transition from inpatient to outpatient environment with housing]
- Intensive Outpatient Treatment with residence (IOP)with residence [Transition from day/night to outpatient treatment]
- Located in the upscale historic district of Hyde Park, and within walking distance of Bayshore Boulevard, this area offers many outside activities to enjoy such as walking paths around Tampa Bay, exercise and fitness stations, local shopping, and much more.
- Hyde Park is 20 minutes from our inpatient program in Plant City where you can still take advantage of our state-of-the-art recreation center, boxing lessons, and fitness program.
- Cell phone and laptop access are available outside of group and program hours.
- Housing is comprised of 4 historic homes that can accommodate up to 32 patients. Each home has its own kitchen, private bathrooms, and a washer/dryer.
- Off-site outings are offered to aid patients in learning to have fun in sobriety. Outings include trips to the bowling alley, the park, and the beach.
- BBQ grills are located throughout the property.
- Patients prepare and cook their own meals (Lunch is catered).
- Basketball and other games and recreational activities are available on-site.
- The property was designed as an open environment within a residential neighborhood and very much feels like you are attending treatment within a home environment with no institutional feel.


Fort Myers DNT Features:
- Day-Night Treatment [Transition from inpatient to outpatient environment with housing]
- Intensive Outpatient Treatment with residence (IOP) with residence [Transition from day/night to outpatient treatment]
- White Sands DNT & Community Housing is in Fort Myers, FL about 25 minutes from the nearest beaches, and 10 minutes from downtown Fort Myers. We are located just a few blocks away from the Caloosahatchee River.
- Each apartment has two bedrooms, one bathroom, a kitchen, living room, laundry room, and bathroom. There are two twin-sized beds in each room, making for a total of four residents per apartment, when full.
- Located 10 minutes from our detox/residential facility and can access spa services such as chiropractic care and can utilize fitness center daily.
- Cell phone and laptop access available outside of group and program hours
- Off-site outings offered to aid patients in learning to have fun in sobriety.
- 12 step meetings nightly.
- Patients prepare and cook their own meals (lunch is catered daily).
- Basketball and recreational activities available on site.
- Property was designed as an open environment within a residential neighborhood with no institutional feel.
- Group hours offsite 8:00-2:15 Monday-Friday with Master’s Level Therapists.
- Weekly individual therapy and psychiatric visits.
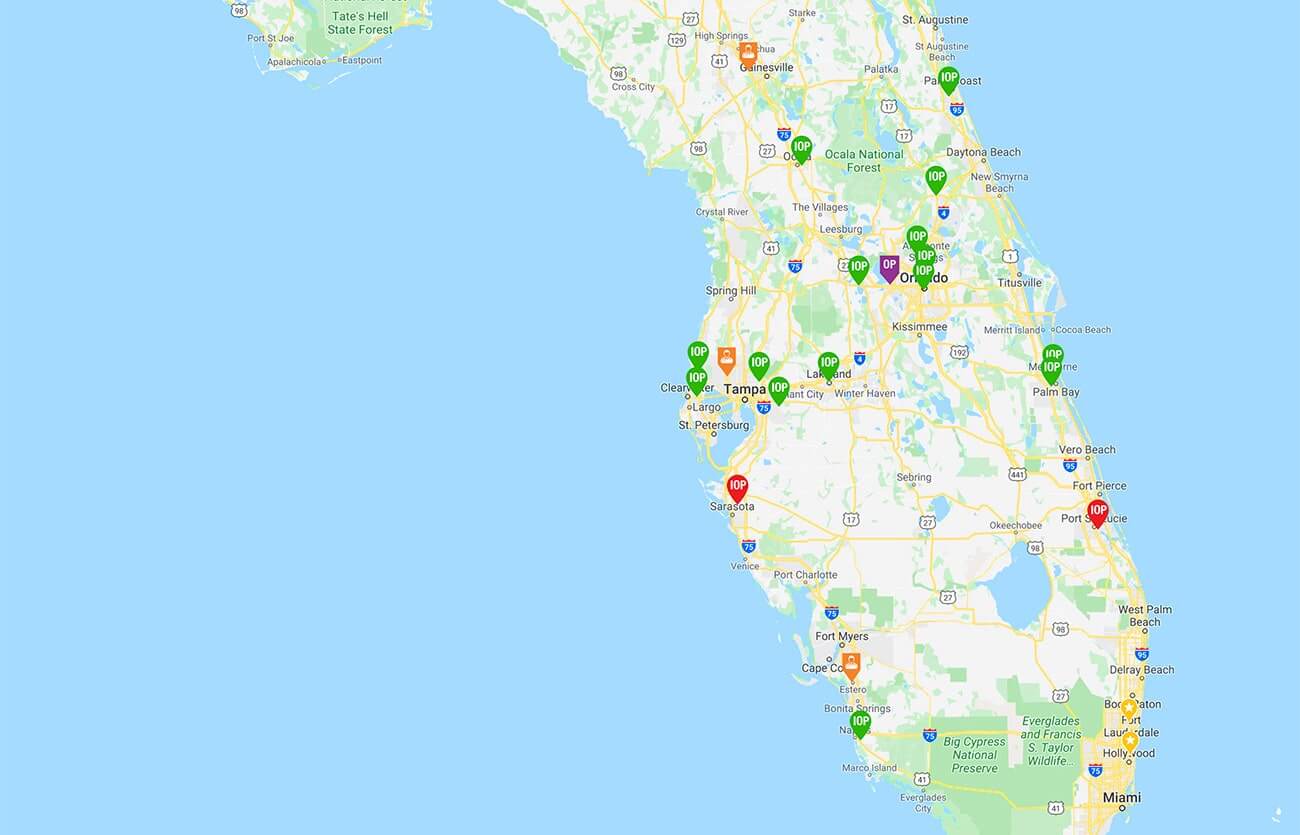

We have 16 outpatient locations located throughout Florida. We do not have pictures of these offices as they are just for meetings and one-on-one sessions. Onsite licensed medical staff and counselors will work one-on-one with patients, assisting and directing them in their journey toward long-lasting recovery. Our outpatient programs offer personalized therapy and individualized care which give patients a network of support during a time of transition, providing ongoing aftercare. When individuals are given the tools and resources necessary to sustain their sobriety post-treatment, they are much more likely to succeed in recovery.
Our 16 Outpatient Locations
Licensed IOP/OP
- Fort Myers
- Brandon
- Clearwater
- DeLand
- Gainesville
- Lakeland
- Longwood
- Melbourne
- Naples
- Orlando
- Palm Harbor
- Sarasota
- Tampa
- Kissimmee
- Ocala
- St. Pete
Accepted Insurances and Self-Pay Rates
We accept almost all health insurance policies so we recommend that you call our admissions department and provide your plan information. We are also proud to service our Military and their families by accepting most Tricare and VA policies.
If you do not have health insurance or your insurance doesn’t cover substance abuse, we offer flexible self-pay rates. We have 3 inpatient campuses and more than 16 outpatient offices, allowing us to devise a treatment plan that fits within your budget. Depending on your particular circumstances, such as the type, frequency and quantity of your drug or alcohol usage, we can design a treatment program that will effectively treat your addiction at an affordable price. Our self-pay programs generally range from $5,000 for one week of inpatient medical detoxification and up to $50,000 for a longer-term comprehensive program. For example, a 35-day treatment plan starting with detoxification and inpatient treatment through outpatient treatment with housing runs $23,000 - $30,000. We also provide finance options for those who qualify. We suggest you call and speak with an admissions counselor to understand your insurance and financial options.
Length of Stay and Program
Your length of stay can vary. In some limited cases, starting at 7 days of detoxification only to up to 90 days including our step down outpatient programs. Typically, our medical and clinical staff recommends a treatment program of 35 to 60 days for successfully maintaining long term sobriety. Our programs are flexible in order to accommodate our guests' particular circumstances. We offer a comprehensive recovery program that includes detoxification and inpatient care at one of our 3 campus-style locations followed by continued care on an outpatient basis. We provide housing options for our outpatient programs. Call our admissions counselors today and they will explain our treatment options.


Admissions Process
If you want to end the destructive cycle of drug or alcohol abuse, it is important to realize that your success may depend on accepting help from others. By recognizing that you have a problem and conducting a self-assessment, you have already taken a crucial step towards recovery. However, it can be dangerous to deal with addiction alone; this often times ends in failure.
At WhiteSands, we are experienced in dealing with addiction and substance abuse. We understand that you initially may have feelings of anxiousness or vulnerability. Our knowledgeable, empathetic staff can help you to overcome these feelings of discomfort as you work towards your goals. Addiction may seem like an insurmountable obstacle, but we’re here to restore hope.
The comfortable, supportive environment at WhiteSands helps to make the addiction recovery process as effective as possible. We provide therapy that helps you to understand the underlying reasons behind your addiction, as well as unique counseling and education for family members. This can help to rebuild troubled or broken relationships that have been negatively affected by the disease.
By conducting a thorough patient assessment, we will be able to identify what sort of treatment modality is right for you.
Steps in the Admissions Process
Step 1 - Call and speak with our admissions counselors
They will ask you the following:
- What is your insurance coverage? Once we know this, we can discuss your insurance plan benefits and self-pay rates, if necessary.
- What are you struggling with? We ask this so that we can understand more about the substance of choice, frequency, and volume of use to determine the specific treatment you require and the treatment options we suggest for your specific situation.
Also, our admissions counselor will answer any questions you may have concerning:
- Our medical and clinical services and programs
- The different types of accommodations and amenities at our 3 campus locations
- Any other questions you may have concerning WhiteSands
Step 2 - Agreeing to treatment and the admittance process
Assuming you want to continue in seeking treatment, we would then verify your insurance benefits with your insurance company. This usually takes about 10 minutes. During that time, we will also conduct a preliminary clinical assessment to understand all of your medical and clinical needs and circumstances in more detail.
Once we have gathered all necessary information, we will then complete the admissions process. If for whatever reason WhiteSands is not right for you or you don’t qualify, our staff will spend the time to review all other options given the information we’ve gathered. We will make every effort to connect you to a facility that will be a more appropriate fit.
WhiteSands Stories of Recovery
















Over 300 Google-Verified Reviews


Rebecca Kutsor
5 days ago“This treatment center is absolutely amazing. I have never felt so safe and loved during such a scary time. The counselors are well versed and very engaged. The accommodations are immaculate and private. The staff are caring and courteous. All of your needs will be met.”


Robert Vannata
5 days ago“Amazing staff, therapists, and doctors. Accommodations are great... Nice rooms, catered food, vollyball, massage, biofeedback, chiropractor, basketball, beach and more. Definitely saved my life!!!”


Anthony Moniz
a month ago“I wanted to stop my habit for a very long time trying on my own never worked I needed help and would never accept it. I finally had enough and gave in to acceptance and looked for help. I found WhiteSands and watched one of the videos they had of a guy around my same age talking about his story and how he found help from WhiteSands. It gave me hope so I ended up calling them and I was there that night. White Sands was a life changer the therapist to the staff all of them played a part in helping me find myself. I’m forever grateful! I’d be dead or in prison if I didn’t get the help I needed. If you read this review your life is worth living. Give yourself a chance to change.”
Kenneth Kaser
a month ago“White Sands is a phenomenal rehab for alcohol and substance abuse addiction. Staff is great! Food is great! They take you on outings, provide chiropractor's, and have a medical staff on clock 24/7. If you're tired and want to give up the fight, then White Sands is the only place I recommend anyone to start! Thank you White Sands!”
Our Most Popular Features
Medical/Clinical Features
Low Patient-to-Therapist Ratio
Our low patient-to-therapist ratio means that guests receive an unparalleled quality of personalized care and support. This also allows patients to build a trusting relationship with their therapist which will further aid in the recovery process. We have highly-accredited and certified clinicians on board that will help guide guests throughout each phase of treatment, from intake to discharge and beyond.
Most facilities only offer large group meetings with limited access to one-on-one counseling and therapy.Full-Time Medical Director and Psychologist On-Site
It is extremely important to us to ensure that help is available when individuals need it most. This is why we have a full-time Medical Director and Psychologist on staff who provide guests with medical support and psychiatric aid; both of which are incorporated into the patient's unique treatment program.
Other facilities will often have a part-time medical specialist and will not always have an office onsite.

Individualized Dual Diagnosis Treatment
Tailored, integrated treatment is crucial for those who struggle with both an underlying mental health disorder as well as an addiction to drugs or alcohol. We offer several treatment therapies for dual diagnosis patients. These include:
- Cognitive Behavioral Therapy
- Behavioral Modification
- Alternative Therapies
Medical Detox Onsite
Medically assisted detox allows clinicians to stabilize and monitor the patient while also managing their symptoms. In our detox program, patients are tapered off of all narcotics under 24/7 medical care and are given additional medications as needed to combat symptoms of withdrawal. This ensures every patient is comfortable and safe during the hardest part of their stay. Read More
Generally, facilities refer detox to a partner, then brings the client back for their stay.

The Detoxification and Inpatient treatment programs at WhiteSands Treatment Center provide services to individuals suffering from alcoholism and/or other forms of chemical dependency and/or abuse. The detoxification program provides patients with safe medical detoxification by monitoring and stabilizing withdrawal risks, bio-medical conditions and complications. The rehabilitation program follows the detoxification program and provides patients with therapeutic interventions, focused on developing and maintaining a healthy recovery from alcoholism and other chemical dependencies.
Whether you are suffering from alcoholism, struggling with a dependence on prescription medication or addicted to an illegal drug like crystal meth, WhiteSands Treatment can offer you a carefully-designed and highly effective program that will facilitate your recovery. Many of our patients need to go through a period of detoxification at the time of admission, and you may be wondering whether this is necessary in your case, and maybe confused about exactly what it will involve.
What is inpatient medical detox?
It is a common misconception that the best way of dealing with addiction is to go ‘cold turkey’; in fact, abruptly stopping a drug is likely to lead to relapse, and could even be dangerous. Inpatient medical detox is a process during which addiction is dealt with by gradually reducing drug dosage. Some of the most common addictions requiring inpatient detox include alcohol, drugs such as MDMA, cocaine, crystal meth, opiate painkillers, benzodiazepines, and barbiturates. Those who consent to undergo inpatient detox for dependence on any of these drugs will dramatically increase their chances of recovery, thanks to the close supervision of medical experts.
At WhiteSands, we have a team of board-certified doctors, nurses, psychiatrists and counselors at our disposal, and a number of these staff members will design and oversee the detox process while providing constant support that helps to preserve your comfort and dignity. Detox begins with a careful assessment of your dependence and an in-depth physical examination that accurately measures the extent of your addiction. We will discuss our findings with you after this, and recommend a precise treatment plan. You can rest assured that we will also let you know exactly what to expect from your treatment and that you will be safe in our hands; we are highly experienced in dealing with physical dependence on drugs and alcohol in a compassionate, gentle way.


Why choose inpatient medical detox?
There are several major advantages to choosing to tackle substance abuse in this way. For one thing, our staff members have received extensive, up-to-date training that allows them to know exactly how and when to reduce the dosage of a drug of abuse in order to minimize the discomfort experienced by patients. Studies show that those who try to stop taking a drug without the help of such medical professionals are much more likely to relapse, mainly because the withdrawal symptoms can be painful and very difficult to handle.
In addition, safety is one of the most significant reasons why we strongly recommend inpatient detox for anyone with a serious addiction problem. Abruptly stopping your intake of certain drugs can be fatal; for example, even alcohol dependence can lead to cardiac arrest if you suddenly stop drinking. You are less likely to experience dangerous complications if you are under supervision while being weaned off drugs or alcohol, and if there are any warning signs of complications during the detox process, then we will immediately notice the signs and compensate for them in order to make you more comfortable. We closely monitor everyone in our treatment center at all times, and we can quickly administer necessary medications to deal with unpleasant physical or mental aspects of detox.
Medication Management
Patients in the detoxification stage of recovery may require medications to assist them in the management of withdrawal symptoms. This includes opioid detoxification, which we are capable of providing, and in addition to that, some patients may need to take medications relating to medical problems on an ongoing basis, while they are participating in both Detoxification and/or the Inpatient Rehabilitation Programs. Medication management is achieved by ongoing assessment by the Medical Director and follow-up by the nursing staff to provide the proper medications to the patients as deemed appropriate to address their medical needs.
What comes after inpatient medical detox?
Although inpatient medical detox is a major step in the rehabilitation process, it is not the end of your recovery. Alcoholics and drug addicts who only submit to detoxification and then stop their treatment will typically show patterns of future abuse. We believe that a customized treatment program involving cognitive behavioral therapy is a vital next step towards recovery, and we offer both individual and group therapy. Our goal is to follow detox by equipping you with the self-awareness and the skills that will help you to understand why you became an addict in the first place and to reduce the chances that you will ever relapse. We also provide family programs that aim at strengthening the bonds that you have with your loved ones by helping them to understand the nature of addiction and helping you to resolve negative feelings that may have emerged during the height of your substance abuse.
Are you ready to end the painful and destructive cycle of substance abuse? At WhiteSands Drug and Alcohol Treatment Center, we offer highly customizable detox programs that are designed to suit the particular drug of abuse. For example, if you are addicted to crystal meth, then inpatient medical detox will be vital to your rehabilitation. However, if you are addicted to a prescription painkiller, then your treatment may be more focused on therapy to combat psychological dependence.
Detox can be conducted on an inpatient or outpatient basis, but we generally recommend inpatient treatment due to the fact that it is more likely to lead to long-term recovery. Regardless of the program to which you are admitted, our board-certified doctors, nurses, and psychiatrists will work to ensure your safety and facilitate your recovery by managing withdrawal symptoms and constantly monitoring your progress in a safe, comfortable environment. By undergoing both detox and therapy, you can expect to notice profound changes in your physical and mental health, and you will leave WhiteSands with the skills to resist relapsing in the future. We also offer family programs that create a deeper understanding of the nature of addiction and help to mend damaged relationships.
Medical Detoxification Program Goals Are:
- Monitor, decrease and stabilize withdrawal symptoms
- Educate patients on the health risks associated with the use of illicit drugs and alcohol
- Assess and treat emotional and behavioral complications exacerbated by the use of alcohol and illicit drugs
- Assist patients in developing an aftercare treatment plan so that they can maintain abstinence in a less restrictive level of care
You deserve to be free from the devastating cycles of drug and alcohol addiction. Call (877) 855 3470 to talk to our team of alcohol and drug treatment specialists about why WhiteSands is the perfect place to recover.
Variety of Groups
At WhiteSands, we offer an extensive variety of groups to patients as part of their treatment program. Some of the groups that we provide are:
- SMART Recovery
- Family Therapy
- Read More
Detox/Res Tampa
- Daily Reflections
- Process Group
- Addiction Education
- Anger Management
- Parenting Skills
- Coping Skills
- Stress Reduction
- Relapse Prevention
- Stress Tolerance
- Family Systems
- Nutrition
- 12 Steps
- Smoking Cessation
- Self-Forgiveness
- Moral Reconation Therapy (MRT)
- Self-Esteem
- Music Interpretation
- Creative Expression
- Mood Management
- Women’s Group
- Men’s Group
- Spirituality and Addiction
- Wellness in Recovery
- SMART Recovery
- Trauma Recovery
- Codependency
PHP Fort Myers
- Daily Reflections
- Process Group
- Self-Reflection
- Dialectical Behavior Therapy (DBT)
- Relapse Prevention
- Coping Skills
- Self-Esteem
- Cognitive Behavior Therapy (CBT)
- Core Skills
- Addiction Education
- Mindfulness
- Family Dynamics
- Codependency
- SMART Recovery
- Meditation
Aftercare/Continuum of Care


Our facility provides patients with care and support even after they have been discharged from their inpatient stay. We offer aftercare programming upon discharge and will set up a therapist and sponsor for them. We have 50 locations throughout Florida consisting of Inpatient, Outpatient, and Admissions Offices, giving patients peace of mind knowing that help is close to home.
Most facilities do not offer as many aftercare and relapse prevention options as we do.Non Medical Features
Private Rooms
Each patient will reside in their own newly renovated private room which is offered throughout the entire facility. The rooms feature a flat-screen TV, queen-sized bed, and a private bathroom which allows patients to be comfortable and relaxed before and after treatment hours.
Other facilities may not offer private room options to their guests.

Cellphones & Laptops Allowed
We offer a lenient cellphone and laptop policy. Patients are permitted to use their electronics in their private room between the hours of 6:30 p.m. and 10:30 p.m., allowing them to keep in touch with family and friends. To protect the privacy of fellow patients, cellphone and laptop use are prohibited in common areas.
Having this feature is very expensive to manage which is why most facilities do not offer this, but we go the extra mile to ensure that our guests have access to their personal electronic devices after treatment hours.10-Acre Campus
Our facility provides spacious accommodations situated on a campus-style site. Having a generously sized facility means that patients will not feel cramped or giving them the space to refocus their minds for further clarity. We offer cobblestone walking paths, streams, and gazebos for patients to enjoy, which can help alleviate the stress that is often associated with this time of change.
The majority of facilities are often confined, hospital-style buildings converted into a facility with no room for amenities.Amenities
Patients can enjoy a host of amenities directly on-site such as a full-size gym, pool, basketball court, and volleyball court. Once your groups are complete for the day, these recreational activities can be enjoyed. We also offer visitation days where the family is invited to the facility to spend some quality time with their loved ones. Weekly outings are an important part of recovery which is why we coordinate fun off-site activities for patients to enjoy.
Most centers do not offer the extensive amenities and activities that WhiteSands does, or does not offer amenities at all.Spa Services
Our facility offers chiropractic care, massage therapy, yoga classes, a full-sized basketball court, and a workout gym for patients to enjoy. Haircut and styling services are also available during patient's stay.
An average facility may only offer one of these spa services. This unique feature is rarely or never offered in a treatment facility setting.Smoking and Vaping Areas
Smoking and vaping are allowed in designated locations throughout the facility grounds, ensuring that both smokers and non-smokers feel comfortable during their stay. Out of respect for all guests attending our facility, patients are asked to strictly abide by these rules.
Some facilities limit vaping, some limit smoking, and some limit both.

| WhiteSands Treatment | Average Facility |
|---|---|
| Low Patient-to-Therapist Ratio | Most facilities only offer large group meetings with limited access to one-on-one counseling and therapy |
| Full-Time Medical Director and Psychologist On-Site | Other facilities will often have a part-time medical specialist and will not always have an office onsite |
| Individualized Dual Diagnosis Treatment | The majority of facilities do not personalize and tailor their treatment modalities to each patient and resort to a 'one-size-fits-all' standardized treatment plan |
| Medical Detox Onsite | Generally, facilities refer detox to a partner, then brings the client back for their stay |
| Biofeedback | Most facilities offer basic, non-progressive or personalized treatment modalities |
| Variety of Groups | Other centers only offer single or limited types of therapy that do not conform to the unique needs of patients |
| Aftercare / Continuum of Care | Most facilities do not offer as many aftercare and relapse prevention options as we do |
| Private Rooms | Other facilities may not offer private room options to their guests |
| Cellphones & Laptops Allowed | Having this feature is very expensive to manage which is why most facilities do not offer this, but we go the extra mile to ensure that our guests have access to their personal electronic devices after treatment hours |
| 10-Acre Campus | The majority of facilities are often confined, hospital-style buildings converted into a facility that has a sterile feeling and no room for amenities |
| Amenities | Most centers do not offer the extensive amenities and activities that WhiteSands does, or does not offer amenities at all |
| Spa Services | An average facility may only offer one spa service. This unique feature is rarely or never offered in a treatment facility setting |
| Smoking and Vaping Areas | Some facilities limit vaping, some limit smoking, and some limit both |
WhiteSands Wiki


What is the WhiteSands Wiki and how to use it
- What is the WhiteSands Wiki and how to use it
- Treatment Offered
- Insurance / Rates / Costs
- A Typical Day at WhiteSands Treatment
- How WhiteSands Was Built Better
- Meet Our Staff
- Our Latest DCF Score & Report
- WhiteSands Compared to Average Facility
- TOOLS FOR ADDICTION RECOVERY
What is the WhiteSands Wiki and how to use it
Click the top right-hand arrow to expand the drop-down menu and select the title of any section to learn more.
Scroll through the different clickable sections on the left-hand side to learn more about our offerings.
The WhiteSands ‘Wiki’ defines, expands, and details the many different aspects of our facility. Each section will allow you the chance to learn more about our treatment center and everything that we offer, from amenities and property overview to treatment modalities, tools for recovery, and aftercare assistance. We understand that extensive research is required when deciding on a treatment center which is why we provide an in-depth and detailed overview of our facility and its features.
Types of Treatment Offered / Recommended



We offer a full continuum of treatment options ranging from medically assisted detox and inpatient treatment services to dual diagnosis and aftercare programs. By offering a continuity of care to patients, we are able to not only monitor their progress and wellbeing throughout the recovery process but also work to foster trusting relationships with our clients which aid in the overall journey toward sobriety.
The evidence-based drug and alcohol addiction programs that we offer have proven to help individuals not only reach sobriety but maintain it. We are pioneers in substance abuse and addiction recovery and take a leading approach that consistently evolves with the advent of advanced treatment modalities. We promise to provide each patient with the best chance to obtain long-lasting recovery from addiction and work with them even after treatment has been completed. We do this by ensuring that patients have support groups and sponsors available near them to maintain their abstinence from drug and alcohol abuse.
Rehabilitation programs focus on providing pharmacological tools, counseling and therapy, and educational resources that are designed for patients' success in recovery. Each patient that has completed their treatment program is invited to join our Alumni where they can continue to learn vital coping skills that aid in long-term sobriety.
Some of the comprehensive treatment programs we offer are:
- Medically Assisted Detox
- WhiteSands Treatment Clinical
- Inpatient Treatment Made Comfortable
- Inpatient Drug and Alcohol Rehab
- Partial Hospitalization Programs (PHP)
- Intensive Outpatient Drug Treatment (IOP)
- Alternative Drug Rehab Programs
- Relapse Prevention and Aftercare Program
- SMART Recovery
- Alumni
Our specialists are available 24/7; call today to speak with a team member to determine what sort of treatment program is right for you at (877) 855 3470. If you are unsure of what type of treatment you require, we have specialists on board who will meet with you to conduct a thorough assessment in order to determine which treatment modality is right for you.
MEDICALLY-ASSISTED DRUG DETOX


The Detoxification and Inpatient treatment programs at WhiteSands Treatment Center provide services to individuals suffering from alcoholism and/or other forms of chemical dependency and/or abuse. The detoxification program provides patients with safe medical detoxification by monitoring and stabilizing withdrawal risks, bio-medical conditions and complications. The rehabilitation program follows the detoxification program and provides patients with therapeutic interventions, focused on developing and maintaining a healthy recovery from alcoholism and other chemical dependencies.
Whether you are suffering from alcoholism, struggling with a dependence on prescription medication or addicted to an illegal drug like crystal meth, WhiteSands Treatment can offer you a carefully-designed and highly effective program that will facilitate your recovery. Many of our patients need to go through a period of detoxification at the time of admission, and you may be wondering whether this is necessary in your case, and maybe confused about exactly what it will involve.
What is inpatient medical detox?
It is a common misconception that the best way of dealing with addiction is to go ‘cold turkey’; in fact, abruptly stopping a drug is likely to lead to relapse, and could even be dangerous. Inpatient medical detox is a process during which addiction is dealt with by gradually reducing drug dosage. Some of the most common addictions requiring inpatient detox include alcohol, drugs such as MDMA, cocaine, crystal meth, opiate painkillers, benzodiazepines, and barbiturates. Those who consent to undergo inpatient detox for dependence on any of these drugs will dramatically increase their chances of recovery, thanks to the close supervision of medical experts.
At WhiteSands, we have a team of board-certified doctors, nurses, psychiatrists and counselors at our disposal, and a number of these staff members will design and oversee the detox process while providing constant support that helps to preserve your comfort and dignity. Detox begins with a careful assessment of your dependence and an in-depth physical examination that accurately measures the extent of your addiction. We will discuss our findings with you after this, and recommend a precise treatment plan. You can rest assured that we will also let you know exactly what to expect from your treatment and that you will be safe in our hands; we are highly experienced in dealing with physical dependence on drugs and alcohol in a compassionate, gentle way.


Why choose inpatient medical detox?
There are several major advantages to choosing to tackle substance abuse in this way. For one thing, our staff members have received extensive, up-to-date training that allows them to know exactly how and when to reduce the dosage of a drug of abuse in order to minimize the discomfort experienced by patients. Studies show that those who try to stop taking a drug without the help of such medical professionals are much more likely to relapse, mainly because the withdrawal symptoms can be painful and very difficult to handle.
In addition, safety is one of the most significant reasons why we strongly recommend inpatient detox for anyone with a serious addiction problem. Abruptly stopping your intake of certain drugs can be fatal; for example, even alcohol dependence can lead to cardiac arrest if you suddenly stop drinking. You are less likely to experience dangerous complications if you are under supervision while being weaned off drugs or alcohol, and if there are any warning signs of complications during the detox process, then we will immediately notice the signs and compensate for them in order to make you more comfortable. We closely monitor everyone in our treatment center at all times, and we can quickly administer necessary medications to deal with unpleasant physical or mental aspects of detox.
Medication Management
Patients in the detoxification stage of recovery may require medications to assist them in the management of withdrawal symptoms. This includes opioid detoxification, which we are capable of providing, and in addition to that, some patients may need to take medications relating to medical problems on an ongoing basis, while they are participating in both Detoxification and/or the Inpatient Rehabilitation Programs. Medication management is achieved by ongoing assessment by the Medical Director and follow-up by the nursing staff to provide the proper medications to the patients as deemed appropriate to address their medical needs.
What comes after inpatient medical detox?
Although inpatient medical detox is a major step in the rehabilitation process, it is not the end of your recovery. Alcoholics and drug addicts who only submit to detoxification and then stop their treatment will typically show patterns of future abuse. We believe that a customized treatment program involving cognitive behavioral therapy is a vital next step towards recovery, and we offer both individual and group therapy. Our goal is to follow detox by equipping you with the self-awareness and the skills that will help you to understand why you became an addict in the first place and to reduce the chances that you will ever relapse. We also provide family programs that aim at strengthening the bonds that you have with your loved ones by helping them to understand the nature of addiction and helping you to resolve negative feelings that may have emerged during the height of your substance abuse.
Are you ready to end the painful and destructive cycle of substance abuse? At WhiteSands Drug and Alcohol Treatment Center, we offer highly customizable detox programs that are designed to suit the particular drug of abuse. For example, if you are addicted to crystal meth, then inpatient medical detox will be vital to your rehabilitation. However, if you are addicted to a prescription painkiller, then your treatment may be more focused on therapy to combat psychological dependence.
Detox can be conducted on an inpatient or outpatient basis, but we generally recommend inpatient treatment due to the fact that it is more likely to lead to long-term recovery. Regardless of the program to which you are admitted, our board-certified doctors, nurses, and psychiatrists will work to ensure your safety and facilitate your recovery by managing withdrawal symptoms and constantly monitoring your progress in a safe, comfortable environment. By undergoing both detox and therapy, you can expect to notice profound changes in your physical and mental health, and you will leave WhiteSands with the skills to resist relapsing in the future. We also offer family programs that create a deeper understanding of the nature of addiction and help to mend damaged relationships.
Medical Detoxification Program Goals Are:
- Monitor, decrease and stabilize withdrawal symptoms
- Educate patients on the health risks associated with the use of illicit drugs and alcohol
- Assess and treat emotional and behavioral complications exacerbated by the use of alcohol and illicit drugs
- Assist patients in developing an aftercare treatment plan so that they can maintain abstinence in a less restrictive level of care
You deserve to be free from the devastating cycles of drug and alcohol addiction. Call (877) 855 3470 to talk to our team of alcohol and drug treatment specialists about why WhiteSands is the perfect place to recover.
WHITESANDS TREATMENT CLINICAL



- Medically assisted detoxification using controlled medications to both ease your withdrawal symptoms and ensure you get a good night’s sleep
- We treat the underlying issues that led you to addiction, not just the addiction
- A higher ratio of therapists to patients, with group sizes averaging from 10-15, which allows for more individual attention
- Multiple group options throughout the day. Not a ‘one-size-fits-all’ approach
- You will also have individual sessions with your assigned primary therapist a minimum of twice per week
Inpatient Treatment Made Comfortable


At WhiteSands Treatment we take a different and less institutional approach to addiction recovery. We understand that it is hard enough to seek help which is why we make the utmost effort to ensure that you are comfortable throughout inpatient treatment. We realize that individuals focus better in therapy when it is not a game of survivor.
We pride ourselves in ensuring that patients are comfortable throughout their time in inpatient treatment. We do this by providing luxurious accommodations that feature a queen-sized bed, flat-screen TV in every room, a private bathroom, and a lenient policy on cellphone and electronics use after treatment hours. By providing a home-like environment, patients feel more relaxed and at ease during a time of change, challenge, and determination.
While we focus heavily on providing the highest quality treatment, care, and support to all patients, we put equal amounts of time and attention into making sure our amenities and accommodations exceed our personal standards as well as the standards of our clients. We are consistently working to raise the bar to provide the best treatment possible coupled with premier amenities and accommodations for our guests.
Knowing which treatment modality is right for you can be overwhelming which is why WhiteSands Treatment provides consistent support to all patients, from the initial evaluation and admittance process to discharge and aftercare. By determining your unique rehab goals, whether that is identifying and overcoming an underlying mental health issue or diagnosing any sort of medical maladies, our compassionate addiction specialists are here to help you through each phase of recovery.
INPATIENT DRUG AND ALCOHOL REHAB


Our inpatient rehab program is ideal for patients who have already been through an inpatient medical detox process. This program also suits patients for whom such a detox was deemed unnecessary.
What can be expected from inpatient rehab at WhiteSands?
Our extensive experience in treating drug addiction and alcoholism has demonstrated that certain medications can be vital in helping some patients attain mental and physical stability. Specifically, we may choose to administer drugs that reduce the cravings associated with abstaining from substance abuse, thereby making your recovery more comfortable and also reducing your chances of relapsing. For example, if you are addicted to prescription painkillers (such as codeine or oxycodone) then medications like buprenorphine and naltrexone can diminish typical withdrawal symptoms. After this type of treatment, you are likely to be more responsive to the programs of therapy that we provide.
When it comes to psychological treatments, we tailor our therapy programs to the individual needs of our patients. We equip you with the skills you will need to cope with life’s stresses, without turning to substance abuse in the future. Through cognitive behavioral therapy, you will also gain a better understanding of why you developed a problem with drugs or alcohol in the first place. We also offer family programs that have a therapy component. These programs are geared toward mending damaged relationships, healing bonds and teaching your loved ones about the highly complex nature of addiction.

Why is inpatient rehabilitation highly recommended?
While many patients are understandably wary of undertaking the intimidating commitment of entering an inpatient rehabilitation program, we believe it is the smartest and most successful way to recover from addiction. What you experience and learn during a short stay in our drug treatment center could prevent you from ever having to return to rehabilitation.
Studies on recovery from addiction show that patients who are admitted to an inpatient medical detox program but refuse to undergo any further treatment, are almost as likely to return to substance abuse. True rehabilitation requires careful, long-term treatment, and that is what our inpatient rehabilitation programs can provide. In a comfortable and relaxing setting, you will receive constant physical and emotional support from our medical team and from fellow members of the WhiteSands community.
Many patients continue to struggle with difficult medical and psychological issues after the detox process is complete, and our inpatient rehabilitation program allows us to monitor your condition and helps to reduce ongoing problems. For example, a member of our psychiatric or counseling team will always be on hand to talk to you if you are feeling distraught, and we may provide you with the aforementioned medications that can reduce cravings or withdrawal symptoms when physical discomfort becomes too difficult to tolerate.
What comes after inpatient rehabilitation?
As you are getting closer to completing the program, you will be assessed once again. At this point, we are happy to help you make a smooth transition back into society by finding a place for you in our sober living community or locating a support group in your area. The goal of such programs is to help you to make a smooth, gradual transition back to independent living. You will be monitored, but you will have more autonomy and freedom than is typically experienced in inpatient programs. You can begin to return to the work and engage in family and social commitments that used to be at the center of your life. Additionally, you will continue to form meaningful, long-lasting bonds with people who have been through similar experiences, and these types of mutually supportive bonds can help to ensure that your recovery is permanent.
Inpatient Rehabilitation Goals are:
- Develop methods of coping to continue to maintain abstinence and psychiatric/behavioral stabilization
- Teach patients relapse prevention strategies and skills to decrease and/or eliminate the cycle of detoxification and inpatient rehabilitation
- Provide patients with methods of coping strategies and skills to deal with unresolved grief, depression and anger issues that may contribute to the patient’s psychiatric/behavioral compensation
- Assist patients to develop aftercare treatment plans so that they can function effectively in a less restrictive level of care
If you or someone you love needs inpatient rehabilitation, contact us today at (877) 855 3470 to find out more about our programs. All conversations are entirely confidential, and our team of experts is more than happy to answer any questions you might have. You deserve to be free from the devastating cycles of drug and alcohol addiction. Call (877) 855 3470 to talk to our team of alcohol and drug treatment specialists about why WhiteSands Treatment is the perfect place to recover.
INTENSIVE OUTPATIENT DRUG TREATMENT


Drug or alcohol addiction can lead to physical, psychological, and emotional damage. While many people struggling with alcoholism or drug addiction will need to be admitted to an inpatient treatment program in order to recover, intensive outpatient rehabilitation can also be highly effective for recovery in certain cases. By moving from inpatient treatment to intensive outpatient substance abuse treatment, you will have the opportunity to gradually transition to being an active, healthy member of society once again. We offer such programs for those struggling with addiction to drugs or alcohol, and we can also help those with a dual diagnosis to overcome their addiction and manage an accompanying mental health issue. You might be wondering, “Where can I find an outpatient drug rehab near me?” But what you should be asking is, “Where can I find an outpatient rehab with high-quality, customized programs that will give me the best chances of success?” The answer to that question is WhiteSands Treatment Center.
What does intensive outpatient treatment involve?
We tailor our outpatient alcohol rehab and detox programs according to the specific needs of each patient based on age, health, history, and other considerations, so we offer treatment programs of varying intensity. However, all of these programs will involve regular visits to the treatment center (often three days a week) and include frequent and in-depth cognitive behavioral therapy. After spending full days in our private rehab facility, you will be able to return home in the evenings. Many of the people in our outpatient programs take part after their therapist has recommended stepping down from inpatient rehab or a partial hospitalization program.

During your time at the treatment center, our professional team of board-certified doctors, educators, nurses, psychiatrists, and counselors will closely monitor your physical and psychological progress, so your treatment program will be continually customized as necessary. In individualized therapy, you will explore the underlying reasons for your substance abuse and learn new coping mechanisms that will reduce the risk of future relapse. Meanwhile, the group therapy program will give you a chance to share stories with other peers who have been through similar experiences, and you will benefit from their wisdom and experience. The bonds formed with other patients in the treatment facility can provide motivation to succeed in rehab and will continue to encourage you to work toward recovery once you leave the treatment center as well.
Assessment and screenings?
Why do we fall prey to drug addiction? Many factors can come into play. At WhiteSands, we will carefully assess your individual situation before making a joint decision about whether you are likely to recover in the context of an outpatient program. Some people may struggle in this type of setting, even if they have been making good progress, and may need to receive inpatient treatment for a while longer. For example, if ongoing problems at home or at work represent a significant part of the reason why you were attracted to substance abuse in the first place, continuing to deal with these triggers while you are away from the drug treatment center may harm you and delay your rehabilitation. The same is true if you might find it hard to stay away from a social group of fellow addicts who do not share your desire to live a sober, healthy life. If you do seem like a good fit for our outpatient programs, you can expect random drug screenings during your treatment. This applies to all of our patients; we want to ensure that all members of the WhiteSands community are continuing to be honest and forthright about their progress.
What are some of the benefits of intensive outpatient treatment?
There are many reasons why particular patients might prefer the option of intensive outpatient treatment. Firstly, there is the matter of cost. Living in a drug treatment center in order to take part in an inpatient rehabilitation program is more expensive than visiting the same center on an outpatient basis. Secondly, outpatient alcohol treatment or drug abuse treatment gives you the opportunity to continue with many aspects of your regular life while working toward becoming sober. You may be able to uphold work responsibilities, you will be able to see your family, and if you are studying to obtain a degree, then this is still achievable while you are in an outpatient program. Thirdly, being able to see family members and close friends can go a long way toward providing you with valuable support during recovery that helps to prevent relapses. Indeed, you can continue to get this type of support while also benefiting from being a part of the close community at WhiteSands, allowing you to have the best of both worlds.
Once you are ready to leave the intensive outpatient program behind, we will help to find support groups in your community and aid you in finding a local therapist. People who leave our intensive outpatient program will be endowed with the types of decision-making skills required to continue to maintain sobriety, and they will receive continued contact from WhiteSands. We are interested in the happiness and well-being of our community members long after they leave the treatment center.
Where Can I Find Outpatient Rehab Near Me?
You deserve to be free from the devastating cycles of drug and alcohol addiction. Do you find yourself or a loved one asking, “How can I find outpatient drug rehab near me?” If so, make the right choice: Call (877) 855 3470 or fill out the form here to talk to our team of alcohol and drug treatment professionals about why WhiteSands is the perfect place to get help from a safe, cost-effective, high-quality outpatient rehab program.
ALTERNATIVE DRUG REHAB PROGRAMS


Alternative treatment programs for drug addiction describes an array of healing modalities other than traditional Western medicine and therapies. Advancements in technology have expanded research parameters that facilitate a greater understanding for different types of alternative addiction treatment.
In some cases, modern scientists have been able to validate the effectiveness of some of these alternative remedies that for centuries has been used to address the symptoms of addiction in different cultures. And, in the last few decades, the holistic approach to addiction treatment that integrates traditional and alternative remedies has been shown to significantly reduce criminal inclination.
The basis for the incorporation of various types of alternative addiction treatment into the rehabilitation process is to provide a wider spectrum of treatment tools to address the myriad of effects that are produced by chronic substance abuse. The holistic approach to addiction treatment achieves this objective through cohesive and comprehensive treatment regimens that can be personalized for a greater number of patients. Another benefit of the holistic approach to addiction treatment is that it veers from the one-size-fits-all drug rehabilitation procedures of the past.
Types of Alternative Addiction Treatment for Drug Addiction
There are many different alternative treatment programs for drug addiction that are available today. Nutritional therapy, exercise, yoga, meditation and biofeedback are some of the most popular with addiction treatment professionals and patients. In fact, for some patients, they are considered to be essential components of their recovery process. Other alternative addiction treatment models that are singularly recognized for their contribution to drug rehabilitation include:
Art Therapy


Art Therapy has been gaining inroads as an effective alternative addiction therapy for the treatment of addiction. Through a process of artistic self-expression, patients are encouraged to explore deep-seated emotional issues that drive addiction and produce symptoms of anxiety, depression and suicide ideation to name a few.
Art therapists employ a variety of techniques that are designed to reinforce self-nurturance and reduce emotional imbalances. Margaret Naumburg, renowned educator and psychologist was one of the first in her field to define art therapy as a distinct form of psychotherapy in the 1940s. In the Art Therapy Sourcebook, Research Psychologist Cathy Malchiodi describes it as a “modality for self-understanding, emotional change, and personal growth.”
Yoga


Yoga is a form of exercise that helps to promote spirituality and a sense of calm, relaxation, and tranquility within the body, mind, and spirit. WhiteSands Treatment employs yoga therapy as an alternative form of addiction recovery and healing. We believe that yoga is a fantastic form of exercise that helps to promote a healthy lifestyle in all aspects of life.
Our certified yoga instructors teach participants certain breathing exercises that can have a significant effect on helping them to concentrate on channeling negative thoughts, worries, or fears that they are susceptible to once they’ve begun to embark on their road to recovery. Yoga helps to address side effects associated with substance abuse and addiction, such as anger, irritability, aggression, depression, tiredness, anxiety, impulsivity, etc.
Chiropractic Care
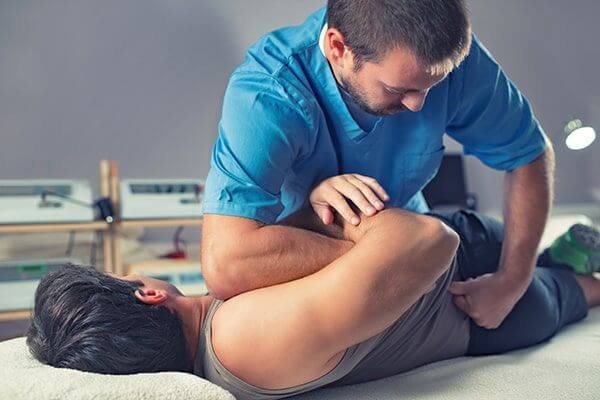

Chiropractic Care is a treatment that involves the manual adjustment or stimulation of the spine, joints, and muscles. It helps with pain management, in which our chiropractors apply pressure to the individuals’ painful areas.
Addiction can often lead to painful withdrawal symptoms and as a result, the threat of relapse is always present. This treatment method helps to ease these symptoms, along with any of preexisting pain that may have contributed to the individual's past drug use.
Alternative treatment programs for drug addiction include various other healthcare practices and therapies that utilize components of Ayurveda medicine, chiropractic services, energy medicine, homeopathy, naturopathy, and traditional Chinese medicine, as well as faith-based recovery tools.
In addition to increased scientific evaluation, the effectiveness of alternative addiction treatments are supported by empirical research and testimonies from patients that have experienced firsthand, their effectiveness through attending our alternative treatment programs for drug addiction here at WhiteSands Treatment.
Relapse Prevention and Aftercare Program


We have several outpatient offices located throughout Florida where patients partake in relapse prevention and after programming. Once inpatient treatment has been successfully completed, patients are encouraged to attend these constructive programs that help teach imperative coping mechanisms and trigger management skills.
We also offer an Alumni program for those who have completed their inpatient treatment program. Our Tampa Alumni Program encourages members to carry on in their life of sobriety. Life after addiction is a major adjustment for many which are why our alumni services work to continually motivate and support recovering addicts to continue in the positive direction they are going.
All Alumni are welcome to partake in ongoing meetings, events, and outings as part of the ongoing recovery process of addiction. Our experienced counselors will provide you with valuable guidance as a way to promote wellness while connecting over stories of strength and hope.
Returning home after your time in addiction treatment can be a hard transition. Let us help you by guiding you on the right path in re-navigating your life.
Call WhiteSands Treatment today at (877) 855 3470 to learn more about the Alumni Program and how to join.
Smart Recovery
Recovering from an addiction is a life-long commitment; it takes long-term dedication and maintenance. It is easy for a patient to fall back into the same dangerous patterns after rehabilitation if they do not remain mindful of their recovery process. Anyone in recovery can fall victim to addiction again, even after years of sobriety. Therefore, it is necessary for each individual to find a way to properly manage their cravings. White Sands Treatment Center provides a variety of programs that give patients access to the knowledge and tools required for life-long success as long as one stays motivated. SMART recovery is a relatively new program that our center utilizes, as it has been proven to deliver positive results.
The Self-Management and Recovery Training program takes a logical, scientific, non-confrontational and motivational approach to maintaining sobriety. Patients who participate in SMART recovery will learn in a highly supportive environment and study methods of recovery that come from evidence-based research. Abstinence from substance abuse is sustained through this innovative and interactive program. Recovery is a constantly evolving process and SMART recovery programs grow with each patient, as they gain more confidence, knowledge, and headway.
SMART Recovery Tools
This 4-point program is a self-empowering support system; primary tools focus on facilitating each patient’s growth through self-management skills, which are tailored to help addicts maintain sobriety from many forms of addictive behavior. Some of these behaviors include alcoholism, prescription, and illicit drug abuse, sexual addictions, eating disorders, and gambling. WhiteSands Treatment Center employs the latest remedial procedures, based on current scientific research and interaction with the community outside of rehabilitation. Our 4-Point Program offers tools for each specific program point. These points include:
- Building/Maintaining Motivation
- Coping with Cravings and Urges
- Management of Feelings, Thoughts, and Behaviors
- Living a Balanced Life
Patients are encouraged to practice each tool, as well as learn how each one can help them progress towards point 4 of the program. The face-to-face SMART recovery meetings offered at White Sands consist of in-depth discussions regarding ways in which to apply the various SMART tools in a practical manner. These discussions may include tools such as:
- Stages of Change
- The Change Plan Worksheet
- Cost/Benefit Analysis
- The Hierarchy of Values
- The ABCs of Rational Emotive Behavior (REBT)
- REBT for Urge Coping
- REBT for Emotional Upsets
- Destructive Images and Self-Talk Awareness and Refusal Method
- Brainstorming
- Role-playing
- Unconditional Self-Acceptance
SMART recovery methods help addicts find independence from addiction through programs centered around scientific knowledge, as opposed to more spiritually based programs. Although SMART recovery may differ from programs such as Alcoholics Anonymous, Narcotics Anonymous, 12-step programs or other self-empowering groups, it does not necessarily exclude them. In our SMART recovery programs, we believe that each individual finds their own path to recovery and here at White Sands, we can help them construct this path. Through self-management and recovery training, achieving lifestyle balance is possible.
Balance your life at WhiteSands Treatment Center. We can help you start fresh and find the support necessary to maintain sobriety through the SMART Recovery program. Take the first step and call us now (877) 855 3470.
Insurance We Accept / Rates / Costs
The cost of treatment will depend on several factors such as the level of care you receive, the length of time you will be spending at WhiteSands, and the type of medical insurance that you have.
Our specialists can assist you in determining your eligibility for our inpatient addiction treatment program. Simply provide us with some detailed information about your health coverage plan by giving one of our treatment specialists a call at (877) 855 3470.
We accept most major insurance plans at our drug rehab in Florida. Our professional staff work with you to ensure that all of your questions as they relate to admittance and treatment are answered. We are dedicated to providing the best care possible to all patients and are here to help you throughout each step of recovery.
Out of Network Insurances Accepted
- Aetna
- Amerigroup
- Anthem Blue Cross and Blue Shield
- Assurant
- Blue Cross and Blue Shield Association
- Cigna
- Coventry Health Care
- EmblemHealth
- Golden Rule Insurance Company
- Guardian
- GHI
- Health Net
- HealthMarkets
- Healthplus
- HealthSpring
- Highmark
- Humana
- Independence Blue Cross
- MetLife
- Medical Mutual of Ohio
- Metropolitan Group
- Molina Healthcare
- Optima Health
- Premera Blue Cross
- The Regence Group
- Thrivent Financial for Lutherans
- UnitedHealth Group
- Universal American Corporation
- UHC
- UMR
A Typical Day at WhiteSands Treatment
Our inpatient treatment program is highly-structured and tailored to the unique needs of each patient. Guests will partake in daily treatment, therapy, and counseling sessions where they will have the chance to open up about their struggles while having the support and care to work through and overcome them. The inpatient program offered at WhiteSands works to stabilize the patient on a physical, emotional, and psychological level so that their recovery goals can be met.
Individuals will be allotted free time every day where they can enjoy many of the sought-after amenities offered directly on the facility grounds. Patients will also enjoy off-site activities as well such as BBQ cookouts and trips to the beach where they have the chance to meet and mingle with others while enjoying time outside of the treatment environment.
Addiction is a complex disease that can be effectively managed with specialized treatment. Each patient who attends WhiteSands will be provided with an individualized itinerary on a daily basis which outlines what their day includes.
Interview With CEO, Garry Jonas
Q: You were operating a successful marketing company, what made you decide to get into the rehab industry?
A: Mike Tyson and I were partners in Iron Mike Productions, which was a boxing promotion agency. Throughout the time spent with Mike, he would often speak about his battles with addiction and substance abuse and the struggles he faced both in and out of the ring. Hearing his struggles made me think, ‘what could we do to help others who are struggling with addiction and substance abuse?’ We then came together to form ‘KO Addiction’; an organization that raises awareness about the growing drug epidemic in the United States. During boxing events, KO Addiction would promote sobriety and provide resources and access to help for those who needed it.
An employee at the marketing company that I had at the time, Joe Ducey, would also speak about his history of addiction and his experiences at different rehab centers. Hearing Mike and Joe’s substance abuse stories resonated with me and I began to realize that substance abuse was extremely prevalent. Joe expressed a significant interest in helping people get into treatment and felt that facilities that truly cared about patients' recovery were lacking. He came up to me one day and asked, ‘why don’t we open up a treatment center’? He knew that the treatment facility sector could use us and with my marketing background and Joe’s history of addiction treatment at various facilities, we knew that we had a great opportunity to succeed.
I sent Joe on a 60-day mission to research what the best treatment centers across Florida offer. If we were going to get into the treatment industry, we were going into it by striving to be the best, offer the best, and raise the bar as it relates to providing the highest quality of treatment to patients without compromise.
Q: How did you turn that idea into the successful treatment center that WhiteSands is today?
A: What it boiled down to was execution: something needed to be done in the addiction treatment industry to make it better and we wanted to be the ones to make it happen. My previous internet marketing experience had its advantages and it gave us an upper hand once the ball got rolling on our idea to create a treatment center that was better than the rest. We were able to hire the best medical and clinical staff without ever sacrificing treatment and the quality of care our patients received. We are successful because we keep the business side of things separate from the medical and clinical side, making us a cut above the rest.
Q: What were some of the things that went into WhiteSands being a premier treatment center?
A: We consistently address our philosophy which is, ‘not cramming in guests like sardines’. We understand that it is hard enough to ask for help and to seek treatment; the last thing we wanted to do was send patients to an overcrowded, crammed facility that strips them of their privacy and space. We make treatment easier and less challenging by providing a campus-style facility for patients during their stay. The large tranquil grounds allow patients to recharge and feel relaxed at the end of the day so that they are mentally and physically rested and prepared to take on their next day in treatment. By providing recreational activities, gazebos, walking paths, and a host of amenities for guests to enjoy, they have a better chance of obtaining long-lasting recovery. We do not make treatment an episode of survivor where, over time, your mental and physical condition worsens. We make sure that guests get better over their course of time in treatment.
Q: What’s the future for WhiteSands?
A: We have opened several office locations throughout Florida such as assessment offices where patients can walk in and meet with an addiction specialist who can help guide them toward recovery. We have also opened several outpatient offices. Once patients have completed their inpatient treatment, they will be sent back to their hometowns where they can meet with a therapist at one of our outpatient office locations so that they can continue to get the help and support needed to sustain their sobriety.
Meet Our Staff
WhiteSands Treatment employs the highest qualified therapists, clinicians, and counselors who demonstrate a combination of credentials and experience in the addiction and recovery field. Our compassionate team works to provide clients with the resources, tools, and support necessary to reach sustained sobriety.
Dr. S. Mann, M.D., Chief Medical Officer, WhiteSands Treatment Center


Dr. Mann currently serves as the Chief Medical Officer and Medical Director of the WhiteSands Treatment Centers and he has held these positions since July 2017. In addition to medical department administrative duties, Dr. Mann is responsible for the medical needs and detoxification of patients at WhiteSands Treatment, Tampa.
Before joining WhiteSands, Dr. Mann has worked in addiction treatment facilities throughout Florida. He has served as an Adjunct Clinical Postdoctoral Associate in the Addiction Medicine Division at the University of Florida, where he enjoyed teaching medical students and medical school graduates during their residency training. He has also practiced Addiction Medicine in the private sector and served as both Medical Director and Associate Medical Director at other substance abuse treatment centers. He currently enjoys both clinical duties and oversight roles as Medical Director of WhiteSands Treatment Centers. Dr. Mann appreciates the teamwork at WhiteSands and how this helps patients resume a happy, fulfilling life.
Dr. Mann graduated with honors from Indiana University where he earned both his Medical Degree and a degree in chemistry. He completed his internship at the University of Miami-Jackson Memorial Hospital before completing his residency in Internal Medicine at Mount Sinai Medical Center in Miami Beach, FL. He later studied Addiction Counseling in Denver, Colorado and he completed an Addiction Medicine Fellowship in the Psychiatry Department at the University of Florida. Dr. Mann is Board-Certified in his field.
Our Latest DCF Score and Report
We uphold to the highest standards of care, treatment, and support, which are reflected by our DCF score. The Florida Department of Children and Families (DCF) is a state agency of Florida and works to ensure that all families have access to the highest quality of services available. WhiteSands Treatment possess the seal of authenticity that shows adherence to ethics and procedures required by an accredited provider.
Our Most Recent Scores:
- Detox/Res Tampa: 98%
- Tampa Outpatient Offices: 100%
- PHP/IOP Fort Myers: 100%
WhiteSands Compared to Average Facility
Not all treatment centers are the same. Take a look at how WhiteSands Treatment fares to the typical, standard treatment center.
| WhiteSands Treatment | Average Facility |
|---|---|
| Low Patient-to-Therapist Ratio | Most facilities only offer large group meetings with limited access to one-on-one counseling and therapy |
| Full-Time Medical Director and Psychologist On-Site | Other facilities will often have a part-time medical specialist and will not always have an office onsite |
| Individualized Dual Diagnosis Treatment | The majority of facilities do not personalize and tailor their treatment modalities to each patient and resort to a 'one-size-fits-all' standardized treatment plan |
| Medical Detox Onsite | Generally, facilities refer detox to a partner, then brings the client back for their stay |
| Biofeedback | Most facilities offer basic, non-progressive or personalized treatment modalities |
| Variety of Groups | Other centers only offer single or limited types of therapy that do not conform to the unique needs of patients |
| Aftercare / Continuum of Care | Most facilities do not offer as many aftercare and relapse prevention options as we do |
| Private Rooms | Other facilities may not offer private room options to their guests |
| Cellphones & Laptops Allowed | Having this feature is very expensive to manage which is why most facilities do not offer this, but we go the extra mile to ensure that our guests have access to their personal electronic devices after treatment hours |
| 10-Acre Campus | The majority of facilities are often confined, hospital-style buildings converted into a facility that has a sterile feeling and no room for amenities |
| Amenities | Most centers do not offer the extensive amenities and activities that WhiteSands does, or does not offer amenities at all |
| Spa Services | An average facility may only offer one spa service. This unique feature is rarely or never offered in a treatment facility setting |
| Smoking and Vaping Areas | Some facilities limit vaping, some limit smoking, and some limit both |
TOOLS FOR ADDICTION RECOVERY
Start your journey to recovery at our Florida rehab center using these essential tools.
Musa Komoni
month agoThis place is amazing. They do exactly what they claim. They get you clean and serene. They have an amazing staff and clinical team. They make you as comfortable as possible. They work with your job and family. They're after care is amazing. This place really cares about its patients they are not after your money believe me. They truly care. I gotta thank white sands for helping me and staying in touch with me to check up on me. I loved every moment here. If you or someone you know is struggling please make the call. Don't wait till is to late
Taylor Jones
2 weeks agoMy sister was in and out of detox so many times that she had almost given up. I told her just call White Sands and give yourself a chance. They got her into detox the NECT DAY and 30 days inpatient, no waiting list....This time when she left it wasn't just a week under her belt. She is still sober today... that tells you about this facility. They care and they help!
hayley zlotnik
a month agoI was here in September of 2017 for 41 days. I am still clean ! I had been to multiple & different unsatisfactory Rehabs / detoxes and I feel this one was the only one that truly digs deeper to get to the route of why I was using. They also made sure that I had a positive follow up plan after I left. I was strongly encouraged to attended A.A./NA meetings and to do 90meetings in 90days.My therapist Kathy was amazing and I was allowed to have family visits where she explained actual addiction and how it works and negatively affect my family members and myself. This helped my dad and I to have a better relationship. He now has a better understanding about addiction and has been a huge support system! I definitely recommend going here for anyone suffering from addiction / alcoholism. We do recover and we don't have to do it alone. White Sands is the only place to go — they even continually follow-up after you leave. Amazing facility and experience.
Joshuah Bean
month agoIf you are reading this wondering if you should seek help or not but worried about the whole process, don't be. White sands saved my life. They made the entire process of getting clean very comfortable. From the time I got off the plane till the end of my stay there, they made me feel comfortable, appreciated, and a part of something much greater than myself. I couldn't of asked for a better place too find myself at. I made friends that I still talk too. Even a few of the staff members have became very close friends to me and I truly appreciate the help and every single person I met through white sands staff or not. Mark ( in charge of alumni) continues too reach out to me asking how I'm doing. Me and him went through this process together and he has stayed in contact with me now even after a couple years. Thank you white sands for the continuous love and support. I will be forever grateful.
Dora Iverson
2 weeks agoThe admissions team made everything so easy. They were knowledgeable, caring and made things simple. I didn't feel judged at all. The clinical assessment was easy and could be done over the phone. Great team! Thanks White Sands!
James Clark
3 weeks agoWhite Sands gave me a new fighting chance at life... From the first phone call...everyone associated with my rehab stay Loved me until I started to Love myself!!! Thank You White Sands♥♥♥
Cameron Easler
a month agoI went to white sands in February of 2017 and I've been to many different treatment centers but white sands was the best decision I had made in a very long time. I'm extremely grateful for them and the opportunities that have opened up for me. I would recommend them to anyone.
Austin Houser
2 weeks agoMy addiction took me to a very dark place to the point where I just wanted it all to end for the pain to go away. White Sands has helped me through my addiction and people reaching out from alumni means a lot.
Jose Velez
2 weeks agoWhite sands treatment talked me through the whole process. Spoke with me the entire weekend prior to admission . Helped me stay inside and stay safe in order to get help.
Mary Falco
2 weeks agoWhitesands has great outpatient groups here and the therapist Alicia is thorough.
caseyann perry
a month agoI've learned a lot with this treatment center, and I feel supported and positive for the first time in a long time!
Chris Green
a month agoJust starting groups here and already happy with the care I have been receiving. Great place!
Dora Iverson
2 weeks agoI would strongly suggest White sands to anyone who is searching for help. This place gave me hope for life when I had none. I never thought sobriety was an option for me and now I see my life totally different. The staff is truly amazing and really does care. The techs are personal and share their stories. The facility was clean and the food was good. I feel fortunate to have been here, and I suggest to anyone looking for help: this is your place.
Joe K
2 weeks agoHighly recommend to anyone serious about transforming their lives. The exceptional & individualized quality of care offered by the White Sands Program is only surpassed by the professionalism, compassion, dedication and knowledge of its entire staff. From the minute I was greeted, I knew I was in the right place. I will never be able to adequately express my gratitude to all of those who guided me on my journey. THANK YOU !!!
Barb McGahey
a week agoThis Facility was fabulous. Awesome program if recovery. Manages dual diagnosis very well. Fantastic, clean , spacious homes. The biggest benefit for me was that nearly all staff are in recovery as week. Great sense of Community. I highly recommend this program to anyone, anywhere.
Samantha Harris
a month agoWhite sands was an amazing place for me. It challenged me and brought a lot of my own issues, not just with alcohol, to light and gave me the tools to better myself and my life. I'm forever grateful for the people I met there and all the counselors/techs/doctors. If you feel you need help, reach out! They're willing and your recovery is worth it. Here's to sobriety.
Ricky Stewart
a month agoWhat a great experience this place was. They have so much support and most of the staff are in recovery. So the team of HELP I got was super authentic in their truth and wanted to focus not necessarily on the drugs but the underlined issues that I continued to struggle with. Great TEAM of Help that support the individual daily and it's not to overwhelming. Any questions I had about recovery, they would gladly share their experience in recovery. Awesome community and the diversity was so powerful in it self. People from all around the United States. Met some great people there and still in contact with them today. Great place and not a 5 star hotel. 5 star staff, 5 star Experience, 5 stars on the HELP I received and a result of my honesty. 5 stars all across the board. Thank you Whitesands. Can't wait to come back and visit.
brandon wienland
a month agoGreat staff and a great facility. In my experience, everything necessary was provided. Excellent care overall with assistance through every step along the way including aftercare and even temporary housing for those that need it. It's daunting trying to find a decent treatment center but they make it easy as possible to get the care you need. It's been 4 years since my visit and they still keep up with me monthly. Highly recommended treatment center as I've referred friends and family there. No complaints from me... Decent food and plenty to go around as well.
Melissa DePerto
3 weeks agoWent here in October 2017 and have been clean/sober since. They will accommodate as best as they can while you are here for your stay. It was my first ever rehab so I was very scared.. I received a lot of comfort from the workers and patients that assured me I would be okay. White sands really left a huge imprint on my heart and I'll always remember my time there. I still have friends to this day I keep in contact with that we're patients there
joyce faragassso
a month agoWhen a loved one goes in for treatment, it can be scary for family members left on the outside. Jay was very hand-holding, knowledgeable, and easy to connect with. He upheld the patients rights to privacy, while navigating the family's concerns along the way in a very professional manner. His care for others well-being and success is evident. This review is written with out hesitation based on our family's experience.
Ang R
a month agoAfter looking into different facilities, I chose white sands, happy I did! The facility and staff are AMAZING! They treat you like a human and not an addict. The counselors are top notch (especially Jeanine) you really get great tools to use once you are out! Anyone looking for treatment shouldn't overlook this place!!
Connie Goins
a month agoI can truly say that my stay at White Sands saved my life. Not only have I been sober for over a year I am happier than I have ever been. I am truly at peace. The staff is amazing and they care. Most are in recovery so they know where you are coming from and what it is like to be where you are when you arrive. When I left after a 35 day stay I was a different person. If you want help and have willingness, this is where you belong.
Federico Herrera
a month agoIt's a very homely facility with amazing therapists. It's dual-diagnosis so they help with getting mentally better as well as chemically helping with rehabilitation from drugs. Definitely not the place I thought I was going but definitely the place I needed to go! I'm a much better person now because of it and I've learned to be a much better and more productive member of society.
Brandon Catalone
a month agoThis place is a Godsend! Saved my life. I owe everything to this facility. Every aspect of this place is OUTSTANDING! I truly did not want to leave. The staff is incredible. Caring. Loving. Sincere. The programs and process they teach is life altering! If you seek treatment, please look no further. This facility is outstanding in every way. A recovery resort of the highest level. Stop your search and call them right away if you seek treatment. They will not only save your life, they will teach you how to live a life in recovery.
James Freel
a month agoWhite Sands is an amazing treatment center. The treatment team individualizes each patients treatment plan. There are various methods of therapy available to patients, each of which is quite effective. This facility not only changed my life but saved my life as well.
Katherine Byars
a month agoWhite Sands was a beautiful and well-maintained treatment center. I have nothing but positive words about the staff, the facility is beautiful and their treatment plans for residents helped save my life. I would recommend anyone who is struggling to seek treatment with this company. Such a loving and helpful environment.
Tim hartwell
a month agoThis is a fantastic facility. The staff really cares. I've never seen a community bond together and unite in such a short period of time. They'll do everything possible to make you comfortable. I'd recommend this dual diagnosis facility to anyone whose willing to create a better life for themselves.
Kevin Carlisle
a month agoWhite Sands saved my life. Every single staff member truly cared about my recovery. Making the call for myself was very difficult but as soon as they answered I began to feel better. Wonderful place to get back to life.
Anthony Moniz
a month agoI wanted to stop my habit for a very long time trying on my own never worked I needed help and would never accept it. I finally had enough and gave in to acceptance and looked for help. I found WhiteSands and watched one of the videos they had of a guy around my same age talking about his story and how he found help from WhiteSands. It gave me hope so I ended up calling them and I was there that night. White Sands was a life changer the therapist to the staff all of them played a part in helping me find myself. I'm forever grateful! I'd be dead or in prison if I didn't get the help I needed. If you read this review your life is worth living. Give yourself a chance to change.
Whitney Rogers
a month agoMaking the call to White Sands for MYSELF & my beautiful, sweet daughter was the best thing I HAVE EVER DONE! FOR MYSELF & for My ‘Duck'. I will never be IMPRISONED to alcohol & INTERNALLY p.m. kill' myself again. White Sands is a PHENOMENAL DUAL Treatment facility, we must fix the root or our reason for using FIRST, IN ORDER to get & stay SOBER. The staff & therapists here are amazingly supportive & informative. You cannot pick a better facility, regardless of what state (Whitney from The 304) to seek & receive the treatment that is needed.
Meghan Sebek
a month agoWhite Sands changed my life!! The staff is amazing. They are some of the best people I've ever met. Most of them are in recovery & can really understand what you are going through. The nurses are so helpful. & the therapists are top notch!! I went into White Sands on September 18, 2016 & I am still sober. I met lifelong friends there. White Sands gave me the foundation for sobriety. I had tried IOP a few times but I needed more structure. I highly recommend White Sands!!!
Ashley Lowe
a month agoDeciding to go to White Sands Treatment Center in Fort Myers, FL was one of the best decisions I made for myself. I had lost EVERYTHING & was SO close to losing my life too. I got connected to White Sands & they got me a ticket to fly down for a 6 week treatment program on January 4, 2017. They gave me tools to use to live a life I deserve & I will be forever grateful for the 2nd chance that the treatment center gave me.
Levi Pinnell
2 weeks agoI have been to two other treatment facilities and had left early because of the lack of care but i have been to white sands a total of 3 times because of the level of care they offer. They have doctors and nurses on staff at all times and BHT's constantly checking on you every 30 minutes so you feel safe at all times and most of the BHT's are in recovery witch helps when you need someone to talk to they are always there for you. The therapists are also very helpful and very professional, the admissions office is also very helpful and the alumni program is also very helpful, if i could give this place 50 stars I would.
Donald Hunter
3 weeks agoI was tired of living my life so lost. So I came to white sands in mid July, and it changed my whole Outlook on life!!! I love myself more, I'm more energetic and positive. It's NOT all about me anymore!!! The groups are a learning experience with counselor's who know what they are talking about because they've been thru it already.. I owe white sands a lot, because of them I get to keep my family!!!!!
Stephan Osmen
a month agoPlace is great where employees truely care came here when I was 24; however I did relapse after and by the time I was ready for help again I had no insurance but felt like I needed a new relocation and reached out to people here at white sands. I couldn't get a bed but they helped me get into a halfway program in the area that didn't require insurance. This is a great place to go and employees will do anything they can to help out all the addicts they can!
James Fike
a month agoI had been through several treatment programs with zero success. I made a call and the next thing I knew, I was on a plane. They were so helpful in every step getting there. I can't say enough about the staff! Understanding, caring, intelligent, etc. (and still are!) I learned so much about myself and my addiction. If not for White Sands, I would not be here. 569 days without any mind altering substance!! My life has changed dramatically! Thanks to all of you at White Sands!!!!!!
Ron Newland
a month agoGreat treatment center, they helped me get my life back on track. The facility is awesome and the people that work there are in recovery so it was so easy to feel like I belong there. Ms.Danielle was a huge support through the process as well. Very grateful!
Hope Ringle
a month agoNever in a million years did I see myself getting clean, white sands did me wonders this place saved my life. The staff are more than helpful they go above and beyond to help you and give you what you need. I'm so blessed to have came to white sands thank you for everything you have done for me !!!
Devon Linge
a month agoApril 1st of 2017 I checked into White Sands. My life was a mess and I was on a path of destruction hurting everyone around me. I was literally on the brink of death and on multiple occasions almost seriously injuring/killing other people while intoxicated. Coming to White Sands I had been to 3 other treatment centers prior but had never received the care I got there. The treatment center is beautiful and the staff are very experienced and caring. White Sands truly changed my life. Without them I wouldn't be the person I am today. I highly recommend White Sands.
Irene Ponnie aka Sadie Brooke Mecham
a month agoHey I'm Sadie I'm an addict i called Ogden regional, Gave them my insurance information and they flew me out to Tampa Florida the next day, they talked to me on the phone, helped me through the airport, I missed 2 planes on the way there and stayed in Houston Texas at a hotel on a layover, I got there, learned a lot, met a ton of amazing people, and discharged to sober living in Cape Coral Florida with an amazing NA system! It all worked great pretty much been sober ever since! :)
KEITH BAKER
a month agoWHITE SANDS changed my life tremendously! It was the best decision I could have ever made. The staff started off as staff but ended up being my family. Don't over think it make the phone call and just go.
Ana Scelza
a month agoMy journey in recovery started with a decision to make a phone call to this center. I didn't know what I was doing. I was fearful. The center walked me through the admittance process with empathy and care. The staff and therapists were top notch. I am so grateful for white sands. -Put the woman together and the world will fall into place. "
Wes Delf
a month agoA friend of mine asked me if I went out one more time. Would I consider treatment. So, I made a phone call to White Sands. I came into detox. They took care of me . I was scared . I got Emily as my therapist. I was presented the MRT work book. That you would have to work through your self to understand. I left 35 days later with more hope and gratitude towards life that I could even Express.
Moriana Cotelo
a month agoThe staff is really nice. They helped make sure I was comfortable and that the facility was as wheelchair accessible as I needed it to be. When I preferred one therapist over another, they allowed me to voice that and switch so I could get the most out of my recovery.
Joe Calabretta
a month agoThis is by far the best treatment facility in the country. It saved my life. I actually feel happy and look foward to every new day instead of waking up dope sick wishing it would end. I have been to 5 different treatment centers and never got any time before white sands. They have a great detox program. I did not feel any withdrawls at all. I was able to learn about myself and why i used and the tools to stay clean after i left. I am coming up on 8 months in a couple days and wouldnt of been able to do it without white sands. The staff genuinely cares and will do anything they can to make you comfortable and help yoy. Most of the staff are in recovery so they know what you are going through and feeling. It is a great facility with excellent counselors. They take you on outings like the beach and park. You can go to AA or NA meetings nightly and they also bring one into the facility as well. It is very clean and the groups are awesome. The food is pretty good. They have a halfway program that you can go to after you complete which i highly recommend. Janette is awesome and actually cares about you and works with you. You can attend Iop too wich is another tool that helped alot. Ask for Kerriann she is a great therapist. Just dont mess with her dog! But foreal i am so grateful for white sands and the time i spent there. I attended it twice cause i loved it soo much! Genuine people who want to see you better yourself and be successful! Addiction is taking too many lives. If you are struggling reach out and get help! You dont have to live like that anymore!
Mark Adams
a month agoI remember how nerve racking it was looking for a treatment center before I found White Sands. I was 22 years old. I had a drug addiction and no idea how to take care of myself or how to cope with life. I was withdrawing from opiates unable to to do the research myself. My sister went on Google and spent hours searching for a reputable center. She found White Sands Treatment Center. The gentleman I spoke to on the phone was very friendly and knowledgeable about addiction and recovery. He was in recovery himself. He clearly explained all benefits of White Sands and also the benefits of getting help in a different area. I Flew from Saint Louis, MO to Fort Myers, Fl to get a new start. The Staff at White Sands was very caring and friendly. The therapists were all very skilled. I learned that each one had their own specialty. I went to their different groups and walked away with different tools. The facility was beautiful. I got my life back admitting into White Sands Treatment Center. I found my self. I found out who I really was, learned how to like and love myself. I Gained confidence and many tools to stay clean and sober. I live a full life today and I thank White Sands for that! I relocated here after treatment and I know work for the same company that saved my life. I am the alumni director. I am able to help others the same way White sands Helped me. I would recommend this center to anyone in need of help!
Kenneth Kaser
a month agoWhite Sands is a phenomenal rehab for alcohol and substance abuse addiction. Staff is great! Food is great! They take you on outings, provide chiropractor's, and have a medical staff on clock 24/7. If you're tired and want to give up the fight, then White Sands is the only place I recommend anyone to start! Thank you White Sands!
Taylor Foley
a month agoWhile I was at whitesands treatment center for 31 days they gave me the option to stay longer if I felt like I needed it, it was an all around amazing environment to get clean. The whole time I was there I was surrounded by people who understood me and comforted me. After my 31 days were up they offered a new environment for me to transition to so I wasn't just thrown out into life and get all mixed up again. My brother followed in my foot steps and also went to whitesands & had an amazing experience. I am now a productive member of society & would recommend anyone to this treatment center!
Jen Gray
3 weeks agoThis facility is absolutely amazing.. Everyone there helped me regain my life back. The staff are the absolute best around.
Pam Offerosky
3 weeks agoI am truly grateful for White Sands, they helped give me my life back. I felt safe and I felt listened to. I learned soo much through the various therapies offered. I have over 20 months clean today and I owe a big thank you to White Sands!! Much love!!!
Samantha E
a month agoI went there at my lowest point in life, and walked out with the tools, support, and knowledge I needed to live a clean and sober life! They literally saved my life!!!! To this day. The alumni team still checks in on me! I've remained clean and sober for 14 months because of White Sands!!!!
Jeff Seacat
a month agoWhite Sands changed my life. It's a treatment center with staff that genuinely cares and wants what's best for you. I'd recommend them to anybody who is struggling with substance abuse.
Brooke Custer
a month agoWhite sands is the 3rd and hands down the BEST treatment center I have ever been to. It opened my mind and my heart to truly recovering, and the staff have experience strength and hope to get you through each day. I loved it so much, it brought me close to New people in recovery, I moved on to their PHP program and am now in their halfway house! I have a job for the first time in over a year and they really still do all they can to help. I know when I'm struggling I can call any of the workers and they are here for me. Thanks White sands! And if you're struggling with whether or not you want to go to rehab, you have nothing to fear. This will become your second home!
Yvette Pryor
a month agoThis place is truly awesome White Sands truly saved my life.. after 3 rehabs my experience was truly awesome here from the treatment on down to the staff was phenomenal I've now been sober for five years with the help. I was very nervous from the time I got to White Sands because I didn't know what to expect but the staff from bhts to nursing to the therapist made me feel very comfortable and relaxed White Sands gave me the tools to remain sober forever grateful that I became a BHT myself at White Sands I strongly recommend this treatment center to anyone dealing with addiction.
Becca Thomson
a month agoI've been to about 15 rehabs and this has been the only place where I was actually able to process my feelings and learn and understand why and what is wrong with me. The facility itself is beautiful and the staff is welcoming.
Lance Douglas
a month agoWhiteSands is an excellent treatment center, not the only one I attended. Very diverse and able to cater to all needs. They dont force feed anything.
Beth Delbrocci
a month agoWhite sands treatment saved my life. I walked through the door and just felt the love and everyone who worked here is so supporting.
brian eddington
a month agoWhite sands helped me in a lot of ways the process was easy the staff were always very friendly and always their to help with anything I needed. Mark the alumni coordinator helped give me the push to get back in here the process was fast I recommend it to anyone who is seeking help.
patrick patton
a month agoThis is the real deal, they do what they say, all you have to do is show up and be willing to commit.the staff is so caring and aware at all times. They make you feel special.
Christopher Wright
a month agoBlessed to have been fortunate enough to go to White Sands. Place is great! Wonderful open atmosphere with a great staff that absolutely cares about its patients.
michael halter
a month agoWell truthfully this place takes away your freedom. Feeds you what they want you to eat. Wakes you up when they want. Makes you go to sleep when they want. Oh and did i forget to mention they take away your fear of getting sober. They help you cope with life on lifes terms. They put a structure in place for the first time in your life. They teach you that its ok to be scared to be sober, and give you tools to cope. They help you look human again by feeding you food that is actually very good. They help you with meds that many of us deny that fact that we need. The best thing this place does is gives you the freedom inside them gates to find yourself and truly connect to others just like us. Thank you so much WhiteSands, and staff for making my stay actually enjoyable.
Kyla Ham
a month agoThe facility was well kept. Housing keeping staff everyday. BHT (behavioral health technician). Very nice always making sure to ask how your day is going. Very compassionate with your recovery. The dr. and nursing staff willing to listen and work with you on any medical issues you have. This place even has a few amenities like chiropractor, massage and a gym. As well as outside trips bowling and the beach. Would definitely recommend whiteSands to anyone looking for help from any addiction.
Maxwell Swanson
a month agoDuring my current stay at White sands treatment center it has so far been the best experience I have had with a rehabilitation facility.
Cody Houchin
a month agoGreat and knowledgeable staff. Very safe place to go if you're struggling. They help as much as possible with aftercare as well.
David Le
2 weeks agoThis place saved my life, I encourage anyone who is still struggling pick up the phone and call white sands. the staff at ft Myers are great people !
Jason Dochney
2 weeks agoStaff and services were very beneficial in identifying and setting a new life to be lived.
Nicholas Bissanti
2 weeks agoI attended White Sands in Plant City in February 2018. My life was on a steep, downward trajectory and I had nothing going for me to speak of. I was a miserable mess, and I had all but completely given up. Thankfully, I found a spark inside me to make the call to get myself into a treatment program. The staff at White Sands was exceptional, making it as simple as possible for me to get where I needed to be. When I arrived there, I was a hopeless mess. I went there without a clue how my life would possibly get any better. I thought I had heard it all before. I have been to multiple treatment centers before, and I got nothing from them. The therapists and techs there treated me like a human being, and talked to me as an equal; rather than trying to drill their ideologies into my head and acting like they knew better, they simply shared their experience with me and told me how they were able to overcome their own obstacles. I was able to relate to them on a personal level, and as a result I became a little more willing to take some of their suggestions. Their approach was very effective for me, much more than trying to listen to authority figures lecture me. After all, I'd spent most of my life rebelling against authority figures as it was! The groups were very helpful. They were not my first introduction to the twelve steps, but this was the first time that anyone had ever conveyed them to me in a way that did not turn me away from them. There are alternatives to the twelve steps as well that are covered in the groups here also. I would recommend anyone considering treatment to keep an open mind to any and all options. I went in there dead-set against the twelve steps, and left with a slight inclination to give them a shot, which has been my saving grace ever since. If you keep an open mind and become willing to try something to better your life, the right path for you will present itself. The living situation at White Sands was much better than I had expected it to be. The location is an old motel that was converted into a treatment center. I shared a room with with one other recovering addict, in comfortable quarters with a bathroom, a TV, and two full size beds that were actually comfortable. Sheets were cleaned weekly. The food was good compared to other facilities I have been to. Many people liked to complain about the food, too much chicken, not a varied enough menu. All very first-world problems if you ask me. As far as I'm concerned, the quality was better than I could've asked for and there was always seconds if you wanted. Some complaints are to be expected from a bunch of addicts fresh off their drugs of choice. Overall, I am eternally grateful. I would not have what I have in my life today if it hadn't been for White Sands. I never thought my life would be where it is today, I am about to celebrate 18 months clean of all drugs and I am on a path to success in my life, the thought of which I had abandoned years ago. I would absolutely recommend this treatment center to anyone thinking they might need help with drugs or alcohol."
Judith Bower
a month agoHaving a son with an addiction problem is a frightening experience for any parent, trying to find the right help is yet another milestone to cross. After combing the internet in desperation and speaking with several different treatment facilities, I came across White Sands. I contacted them and actually spoke with a REAL person immediately. The initial woman I spoke with was very understanding and took all my information; she then transferred me to a gentleman named Jay Redding who immediately worked on getting my son the help he needed. He told us to bring our son in right away to start his treatment. I couldn't believe what I was hearing. He stayed on the phone with me for what seemed like hours, listening to my story and offering all the help that White Sands had to offer. Jay continued to keep in touch with me and was always there to answer any question I had regarding the program. If he didn't have an answer, he made sure he put me in contact with someone who did. Their 28 day program was amazing. Our son was constantly monitored during the Detox phase, saw Doctors and Nurses frequently, and was made as comfortable as possible. Their Therapists and Counselors were all top notch and really cared about helping their patients recover. The best part was, our son really liked the program, put in the hard work, and seemed to be flourishing there. As the program came to an end, we knew coming home was NOT an option for our son. Once again, I knew I could count on Jay to lead me in the right direction. Jay suggested that I contact Recovery Life Homes in Cape Coral to see if we could get our son into their Sober Living Community to continue the help and reinforcement that he still needed so badly. I cannot say enough about Janette Lopez and her program. From the second I spoke with her I knew we were in good hands. She too spoke with me for what seem liked hours, answering all my questions, listening to me cry, and assuring me that our son would be okay. She truly cared. This complete stranger has been nothing short of a Godsend to our family. We enrolled our son in her program and he continued to work on his recovery daily. I cannot say enough about her and her amazing team of Therapists and Doctors. Janette is a caring and dedicated person in helping these men and women on their journey to recovery. Our son lived in her sober living house for 3 months and has now transferred, with the help of Janette, to a long term recovery program. Had it not been for White Sands and their team of extraordinary and caring individuals, I don't know what we would have done. They truly have all the tools and programs necessary, from the initial Detox, to long term programs to make recovery become a reality. Thank you all from the bottom of our hearts. You saved our son. Judy & Glenn"
Joshua Noyes
a month agoThis place turned my whole life around... Great place to learn a new way of life
A. D Cypress
a month agoGive this place a chance! Be open minded, it works! Bring patience!
Kate white
a month agoForever grateful to find this new way of life thanks to this facility. I would recommend white sands to anyone struggling with substance abuse.
Brandon Meece
a month agoIt was a great learning experience and the staff and people there couldnt be more supportive. I couldnt have asked for a better treatment center and the staff and folks who are in the program couldnt be more insitive. They truely get what we are going through and always treat their clients greatly
Jason Douglas
a month agoWas the best decision of my life was to go to White Sands. I struggle with meth and a close call with suicide. The moment I was placed in touch with the counclers thier they walked me threw every step, even when I wanted to back out of getting on the plane. They were very supportive. I thought I had lost everything in my life but with the counseling and the constant support I have learned to break my addiction and learn to love my self again. I will never forget the love and compassion that all the staff had for us there. Thank you again White Sands for giving me back.
Adam Schwartz
a month agoI checked into white sands on June 10th a complete mess from alchohol today is day 23 and im completely changed and sober tomorrow I'm off to php for 10 days and can only say white sands saved my life thanks Morgan Brian and mike for all your help
Darrius Mitchell
a month agoMarch of 2017, I picked up the phone at 1am and called white sands. Tired and broken from trying to keep up with my addiction. From the moment Tom answered the phone, yep I remember the agents name because on that phone call he helped me not only start to accept that I had a problem he helped me make the decision to change my life. Since I live close to the center they had a taxi pick me up the next morning!!!! For the next 41 days I went through a program that saved me. I was 23 when I went to whitesands and i met people from all over the country. Young and old. It felt like a huge family. Everyone helping each other to survive and learning how to handle your disease. I've lost most of my family to addiction and I'm not letting it take me. The staff, the nurses, the counselors all are amazing. One thing that really hit me hard was that the majority of the staff are also in recovery!!! Most of them with decade years clean. Older and younger staff, someone for anybody to relate too. Please if you need help call them and let them help you. Dont wait to get help. Best decision I've ever made was calling the number posted right above this post!!!!!!!!! ♥♥♥♥♥♥
April Randes
3 weeks agoWhite Sands was the very beginning of my recovery that is changing my life and only for the better! The majority of the staff are also in long term recovery and that meant alot, only an addict gets another addict. I was welcomed, cared for and felt comfortable for 30+ days! Rooms are hotel rooms that are taken care of daily. I have only positivity from White Sands..my family was able to visit weekly. White sands provided cigarette runs multiple x a week also Walmart shopping lists for us if in need of any belongings. Our meals were prepared and catered 3x a day and yes, we gained some weight..lol
I owe my sobriety to White Sands and I look forward to visiting and speaking there in the near future!!"
ANNE-MARIE EPISCOPO
a month agoWonderful place. The counselors and staff really do care about you and are always there for you.
jennifer toschak
a month agoThis place has saved my life!! A beautiful facility and amazing staff!
Tyler Goldsborough
a month agoInpatient was very nice and clean and very helpful staff
Andrew Schulz
a month agoGreat place to seek help if you're dealing with drug and alcohol addiction
Pam & Lynn Court
a month agoWhite Sands Treatment Center saved my sons life.
Matthew James
a month agoThis place provided the gateway to hearing a message that saved my life that i continue to apply on a daily basis, going on 3 years now ..
deb meyer
a month agoHelped me with chronic pain.
Rebecca Kutsor
2 weeks agoThis treatment center is absolutely amazing. I have never felt so safe and loved during such a scary time. The counselors are well versed and very engaged. The accommodations are immaculate and private. The staff are caring and courteous. All of your needs will be met.
Jeanne Huber
3 weeks agoI was in desperate need of help as a recovering addict who messed it all up. When I called, I was given a kind listening ear, great information, and the red carpet treatment in getting me here, admitting me and making my stay as comfortable and healing as possible. The staff, doctors, and counselors are professional and give great service. I love it!
John Franco
2 weeks agoWhat a great place to get back on track. I was in desperate in need of help. I was not sure how or where. When I called, the customer representative was very kind and understanding. The place was just perfect and the staff were friendly. I am now getting to be in a better place in life and I thank White Sands for being there to help me.
Patty Doyle
3 weeks agoThis place seriously saved my life! The staff is all amazing and listen when you need someone to talk to and have taught me great tools to stay sober! I met the most amazing people in here that I still see today. Thank you for everything you do!
Terrisha Carr
3 weeks agoI traveled across the US to whitesands for treatment in April 2018 and I am still clean today! I will forever be grateful for this place for helping save my life! Amazing staff, plenty activities, and clean fun environment. From admissions to discharge everyone works together and shows they genuinely care about the patients. I will forever recommend WhiteSands to anyone struggling with addiction!
Adam Hogan
3 weeks agoI feel like this place saved my life. The entire staff makes it evidently clear that they are heavily invested in their jobs, many have even dealt with/are motivated by addiction issues in their personal lives/immediate family. They have doctors and nurses constantly on staff and have medically assisted detox to help people through the initial week or so. I loved the majority of the therapists but a minority can be hit or miss. The majority of time is spent in group therapy which I found very helpful. The center itself is a converted motel with private rooms and a pool that isn't too unfamiliar. My only complaint would be about the cleaning staff sometimes taking short cuts but if that is the only complaint it could be much worse.
Donald Moats
a week ago-I am so very grateful for White Sands and the amazing, wonderful and ever so caring staff. They have been instrumental to my recovery. They saved my life!! The house Keeping staff were wonderful and kept my room spotless, The therapist's and counselors were all different in thier teaching methods which exposed me to a wide array of endless possibilities of help. The only compaint I had is that I finished the program and had to leave, They were wonderful.
Sabi Mariana
3 weeks agoWhite Sands truly helps people desperately needing recovery. The staff is amazing and caring. If you or someone you care about is suffering from addiction, I highly recommend you send them to this facility. You won't be disappointed.
James Clark
3 weeks agoI was desperate and on my last leg when I reached out...from the initial phone call thru my departure... I was treated with compassion and respect... admissions..BHTs...nurses...doctors...therapist and discharge were all terrific!!!! The facility is an extremely comforting setting. I would recommend that if you are struggling...make the call...they can help you save your life...Thank You White Sands for giving me back my life♥♥♥♥
Shawn Galvan
a month agoVery great staff. Friendly. very professional. Best help in swfl
Marc Wilson
3 weeks agoTruly blessed to find this program. The staff and therapists are amazing. I recommend this program to anyone struggling and looking for help. White Sands saved my life!
braxton haley
3 weeks agoWhite sands was a wonderful place. The staff is excellent and can relate to the clients on a different level. I'm grateful for this place in so many ways.
Robert Vannata
3 weeks agoAmazing staff, therapists, and doctors. Accommodations are great... Nice rooms, catered food, vollyball, massage, biofeedback, chiropractor, basketball, beach and more. Definitely saved my life!!!
Issac Martin
3 weeks agoVery great experience there, all of the staff was very welcoming! There was not a single let down while I was in treatment there and I was provided with all the tools necessary to go on with my new season of life.
Austin Hancock
3 weeks agoWhite Sands saved my life. Desiree in admissions has helped me tremendously in my recovery. I would recommend this program to any struggling addict.
ember johnson
3 weeks agoThis facility might not look the best but the quality of care and treatment is exceptional. If you are looking for a treatment center I would definitely come here.
Scott Harris
a month agoI'm am so glad I chose WhiteSands fir my recovery. The staff is wonderful and the experience over all was awesome.
John Brown
2 weeks agoSafe and comfortable detox with a very knowledgable staff
Ashley Phillips-Jimmie
3 weeks agoThis place has saved my life and without the help of everyone here and all the work I'm putting into my recovery I wouldn't be where I'm at today. THANK YOU to everyone!!!!!!
Mike Zappitelli
2 weeks agoaddict that was in desperate need of help. Got the help i needed
Nicole Zhang
2 months agoMy wife and I completed the program there. It was amazing and the staff was also amazing. This place saved my life and my family.
Rebecca Flores
month agoThe staff at White Sands saved my life. Their staff is very caring and available to speak with when needed.
Katie Vance
5 months agoIf it wasn't for these guys I wouldn't be where I am today. Addiction doesn't only hurts you but it hurts everyone around you as well and being induced with drugs you fail to realize that. I can't thank you enough for saving my life
Amy Adams
4 months agoI was sick when I went to WhiteSands, and they helped me in every way to get through my addiction and help me recover. Thank you, for all you have done in creating a special place for healing and recovery.
Brooke Johnson
5 months agoWhiteSands of Daytona Beach is definitely the best Drug Rehab Center in Florida. Thank you for helping my son get back on his feet!
James Clark
a month agoWhite Sands truly saved my life!!!
Adam Schwartz
month agoCame in 33 days ago a mess and I have to say the admissions process was a breeze they do drug test and give a breathalyzer but dont be afraid of it it's just to see what they need to treat but now I'm a different guy and feel great the fortmyers facility is beautiful and the techs are great thanks Morgan Bryan and everybody else I had contact with
Jenifer Bolen
month agoAdmissions was smooth and easy. They got me into inpatient treatment the same day
Angel Haslam
month agoVery helpful staff
Rick Jordan
month agoGreat staff
Sheena Glover
4 months agoMy daughter is a young professional who struggled with addiction. She entered WhiteSands of Fort Pierce few months ago and received an excellent course of drug rehab. Her therapist was exceptional, she returned my daughter to a happier & a healthier version.
Tessa Allen
2 months agoIf you wish the inimitable Rehab Center all-around, you ought to employ WhiteSands of Fort Pierce. WhiteSands is one of the best rehab center in Fort Pierce.
Debra Jeter
4 months agoMy experience at WhiteSands was phenomenal. Everyone on staff was so loving and caring for our needs. I learned how to get clean and stay clean through this place. Such an excellent facility and hardworking staff.
Paula Cooper
4 months agoThis is a wonderful place. The staff is great, open, and communicative from the very being. Thank you WhiteSands for saving my life.
Heather Esparza
4 months agoThe counselors were non-judgmental and quite experienced in the field of alcohol & addiction treatment. It was a valuable experience overall.
Kimberly Willard
4 months agoI just wanted to say that everyone was amazing and kind and in my opinion, they genuinely care about the "job" they had taken on.
Tia George
4 months agoThe drug addiction treatment center is quite a place. The staff truly cares and endeavors to help individuals in need.
Erin Martin
4 months agoWhiteSands is a great facility in Fort Pierce. They make sure you recover and work hand in hand with you.
Jill Waltemeyer
4 months agoThe people that work in this alcohol and addiction treatment center are sent by God. They go above and beyond for you. This place saved my life and gave me another chance to live. I owe it all to them.
Donald Hunter
3 weeks agoThe admissions staff was friendly and the process was quick and easy and the ladies were super hott!!
Julian Koenig
2 weeks agoGot me to the facility as quickly as possible, still keeping in mind my personal life. Everybody that I had talked to on the phone beforehand were super helpful and made me feel comfortable about doing it, being my first and hopefully only treatment.
Tyler Camp
2 weeks agoWhite Sands Has an overall great staff! I had a great experience. Thank you to all the staff
Rocco Pompeo
2 weeks agoThis place helped in one of the darkest moments of my family's history. They cared and were always so easy to talk to through the entire admission process.
Arianna Owens
2 weeks agoThe best quality about white sands treatment center is they are alwayd wanting to help and will bend over back wards to do so. I was admited into fort meyers treatment the same day that i called amd was successful for 60 days. And being alumni i thought after i relapsed that i wouldnt be priority to come back. But as soon as i called everyone was overjoyed that i wanted t come back and got me in the nect day. White sands understands that you domt always get it on your first try and are willing and happy to help us in any way possible along our recovery journey.
Jason Cameron
a year agoWhen I arrived at this Naples Rehab Center, I was lost, broken, shamed, and felt as if I was a complete failure. With the help from this center, I felt understood. I felt comfortable. They gave me the tools to succeed. And live a happy, healthy lifestyle. I went through the program and it helped me further my focus. I've never felt afraid to say how I truly feel. And to process those feelings. It's hard work but that's apart of life. Sometimes you have to accept defeat. I've always felt welcomed with open arms. It's an amazing experience. I would recommend WhiteSands Treatment Centerto anyone struggling. Thanks again for saving my life. You guys are family to me.
Joe Meziere
2 weeks agoMy wife called in to get me help. They werw always nice and helpful
Mary Falco
2 weeks agoBeneficial one on one groups i got alot out of the program
Jessica Quiles
2 weeks agoI can't thank white sands enough for all of their help with my loved one. Amazing place!!
Phillip Lopez
2 weeks agoVery quick and informal. Caring individuals
Ron Newland
a month agoThank you so much for helping me through the process to get the help that I need and for the continued care.
Hugo Fowler
10 months agoA friend of mine went to this drug addiction treatment center, more than one and a half years prior. This person has been clean from that point forward. WhiteSand Treatment Center saved his life. I am extremely grateful!
Patti Vineyard
3 weeks agoWorking with Susan has been extremely beneficial. I highly recommend her program.
Amberlyn Hauck
a month agoMy sister has worked here for over 3 years and she absolutely loves it. She is able to spend her time helping making a difference for so many people!
Ericka Zhang
4 months agoThe staff is incredible and knowledgeable about addiction treatment. The ambiance is stunning and I would profoundly prescribe it to anybody needing help.
Lance Floyd
10 months agoIt is a wonderful place for addiction treatment in Gainesville. I loved it. Great staff and it changed my life for the good. The staff and therapist care about you.
Julian Bennett
a year agoMy sister has been an alcoholic for many years and it was clearly taken its toll on her body and mind. We called around and spoke with many centers before deciding on this drug rehab Gainesville . The Treatment Center staff was straight forward, honest and most helpful. I never thought i'd see the day my sister was alcohol free but that day came with the help from all the staff at the center. We couldn't be more grateful to them for all they have done for our family having my sister back, thank you all so much!!!-+1*
Scott Harris
a month agoThis place is awesome. I am an alcoholic that relapsed after nine years of no drinking. I am confident that the treatment I got from WhiteSands and the tools they've provided will keep me alcohol free for the rest of my life. The staff is excellent. The living quarters are magnificent. Five stars all the way!
Alicia Patrick
a month agoWhite Sands beat all expectations we had. They truly helped my friend address the origin of her issues and turn her lief around. The care and dedication they showed is what we appreciated the most. Though it was a touch situation to be in, they made the experience pleasurable. Thank you!
KALI STUBBS
a month agoMy cousin had the most wonderful counselor. She absolutely saved his life and we are forever grateful to them. I will never be able to describe in words how much this means to our family.
Shawnda Head
4 months agoI went to this drug treatment center for help. My first day at the drug rehab center, I knew this was not only where I had to be but where I wanted to be. I was welcomed like family not only by the staff but by the clients as well. It made it easy to get settled in. The staff was amazing, great people. I miss every one of them. WhiteSands really does go the extra mile when it comes to helping clients. I am forever grateful and I am so thankful to meet each and everyone one of you, thank you for everything.
Brooke Campbell
4 months agoSafe, comfortable environment with an excellent group of people. I trust and recommend WhiteSands of Sarasota to those in need. Your friends and family members will also leave with hope and positive emotions.
Lauren Melendez
4 months agoBest alcohol and addiction treatment center in Sarasota. They are making lives better.
John Burress
a month agoAmazing facility, really professional and friendly staff
Chuck H
a month agoI highly recommend White Sands
Andrew Wolff
a year agoThe staff at this Sarasota rehab center were amazing and so helpful. They kept me informed of the problems and the progress through phone calls and emails. This program saved my son. I will be forever grateful to everyone that played a part in his recovery.
Lori H
a month agoWhite Sands is amazing
Becca Thomson
a month agoThe admissions process was simple and they kept in contact with me until I was ready which was four months back and fourth. I was also going to go to another place and they weren't mad or pushing me to come here. The staff are the nicest you will ever meet.
Tim hartwell
a month agoThe staff really makes an effort to guide you through the administration process as you make your way from your respective area to the facility. The amount of empathy felt before even meeting anyone was amazing. I'd recommend this facility to anyone.
Moriana Cotelo
a month agoThe admission process was pretty simple. They called me back pretty fast and told me what to expect and then had someone meet me as soon as I pulled into the parking lot. It was a pretty pleasant process, actually.
Federico Herrera
a month agoSo helpful! I'm from Ohio and they guided me the whole way down to Florida! They helped get me a flight the same day and a taxi to the airport as well. They were very reassuring that I'd be ok and were very empathetic and caring and helpful in every way!
Cody Houchin
a month agoGreat and knowledgeable staff. Very safe place to go if you're struggling. They help as much as possible with aftercare as well.
Robert Vannata
2 weeks agoGreat staff. Good program.
Mary Viereck
4 months agoThis people understand the gravity of situations and treat accordingly. Best drug rehab center in St Petersburg.
Monica Broussard
4 months agoRecovering from the damage and trauma an addiction problem cause can be painful. However, you guys have made what seemed a near-impossible task a reachable one. Thanks.
Alejandro Graves
9 months agoWhen I arrived at this drug rehab center, I was hopeless, broke, and helpless. I cannot believe I am walking out as a completely changed man. Full of life and hope that my future will be bright. Thank you WhiteSand Treatment Center. You gave me my life back.
John Burress
a month agoThe Sarasota location referred me to this location and I could not be happier with their service.
Denise Holloway
10 months agoThe staff go above and beyond in ensuring that all the patients get the treatment they need. Best drug rehab center in St Petersburg.


Meet The Team
WhiteSands Treatment employs the highest qualified boxing trainers and instructors who demonstrate a combination of credentials and experience in the boxing and recovery field. Our compassionate team works to provide clients with the resources, tools, and support necessary to reach sustained sobriety.
Nelson Lopez Jr., Boxing Instructor, WhiteSands Treatment Center


Nelson Lopez was born and raised in a boxing/karate family where these competitive sports were a large part of growing up. Some of his accomplishments include competing in the Florida Golden Gloves Champion ‘98 and ‘99 and representing Florida in the Super Heavyweight Division in Biloxi, MS.
In 2001, Lopez received a Bachelor’s degree in both Science as well as Psychology from Nova South Eastern University. He began his career as a biology teacher at his hometown high school and worked as a strength and conditioning coach for the basketball and football teams. After practice, he would open up his gym where he trained many amateur boxers and world champions alongside his father.
He started the first amateur team in his hometown in 2002. He worked at widening his network and went off to travel the world as a trainer for Olympic teams and various regional teams. Lopez then ventured into managing fighters and matching fights all over the world which allowed him to develop long-lasting relationships with many top-level promoters.
He developed a passion for this beyond just the desire to win and earn money, but the desire to change lives and give opportunities to those that needed it most. Lopez targeted the fighters that lived in the poorest countries and brought fighters from all over the globe to the U.S. to compete. By virtue of this opportunity, the move helped them feed their families, build their homes, and develop their small businesses back in their home countries. These fighters are forever thankful and Mr. Lopez is grateful that he had, and continues to have, the ability to help. “I want to pass my knowledge on to the patients/guests of WhiteSands Treatment Center and teach them what boxing taught me: discipline, determination, and respect. With this, anyone can conquer anything”.
Asa Beard, Boxing Trainer, WhiteSands Treatment Center


Originally from Manchester, England, Asa is the youngest of 13 children. Asa started playing soccer from the early age of 4 and did some martial arts as well, but always stuck with his two main passions: football and boxing. Asa has trained athletes of all levels in multiple sports such as soccer, boxing, and personal training, and at the age of 16, began training fighters where his huge passion for the art of boxing grew stronger. He was eventually asked to train some fighters in his hometown after becoming a professional soccer player. He graduated from college with degrees in Business, Personal Training and Leisure, and Tourism and is an expert in fitness and nutrition.
Asa has worked alongside some of the best in the business, training and coaching with some of the most respected trainers in the world. Asa has worked with world champions and former world champions, as well as training and developing some amateur fighters in his own youth soccer club.
Asa trained alongside Floyd Mayweather, Sr. Roger Mayweather, and Jeff Mayweather while in training camps with his fighters. Asa was invited to train and work alongside hall of fame fighter, Manny “Pacman” Pacquiao and trainer, Freddie Roach.
Upon moving to the United States, Asa spent time at the Mayweather Boxing Club, Wildcard Boxing Club, Top Rank Boxing Club, Amir Khan Boxing Club, Kronk Gym, and the Phoenix Camp for many years where he was able to fine-tune his trade as a coach.
Asa’s extensive knowledge of the game, and his connections in the pro athlete community, make him an invaluable asset. His years as an athlete have given him priceless insight and understanding of the sport. Asa’s fast hands and intense coaching skills have gained international respect from some of the best fighters in the industry.
After spending time at some of the world's top-ranked gyms, Asa now lives in Tampa, Florida with his wife and children. He has always had a passion to help others and give back to the community which has made him an exceptional addition to the WhiteSands team. Asa is very excited to be a part of WhiteSands as a boxing trainer and looks forward to continuing to help positively change lives.


Services and Program Details
At WhiteSands Treatment, we offer a full continuum of treatment programs and services. Our goal is to prepare you for your own unique journey toward recovery and to provide you with the tools, insight, and support you’ll need to achieve lasting sobriety and avoid relapse. Some of the services that we provide are:
- Individualized programs
- Moral Reconation Therapy (MRT)
- NA/AA
- Smart Recovery
- Multiple group options are offered throughout the day
- Individualized treatment planning
- Multiple individual sessions per week
- Family therapy
- Family visitation is offered weekly or by special request
- Smaller group sessions
- Licensed primary therapists
- Complete history and physical within the first 24 hours of admission to WhiteSands
- Extended slow tapers off of all mood and mind-altering substances
- Licensed Nutritionist reviews and approves all menu options
- Full-time dedicated staff
- All vitals are monitored throughout the course of the day for your safety and comfort
- Full psychiatric assessment within first 48 hours by Board Certified Psychiatrist
- Follow-up psychiatric assessments once a week
Services and Program Details
-
Individualized programs
When you go to treatment, you will often find that most centers offer one type of program, which is certainly easier and cheaper, but may not fit all of the patient’s individual needs. At WhiteSands we want you to have the flexibility to choose the program that best fits both your personal preferences, and any underlying issues that exacerbated or led to your addiction.
-
Moral Reconation Therapy (MRT)
MRT is a Cognitive Behavioral therapy-based program that addresses the underlying issues related to addiction and life struggles. This allows us to provide more in-depth treatment and not just place a “band aid on the bullet hole.” We have multiple counselors that are trained and certified to conduct MRT groups so that everyone participating gets the one on one attention needed.
-
NA/AA
Known as Narcotics Anonymous, Alcoholics Anonymous and the 12 steps
-
Smart Recovery
Smart Recovery is essentially the principles of NA/AA without the higher power component built into the philosophy.
-
Multiple group options are offered throughout the day
Patients can select groups that best fit their personal needs after consultation with their primary therapist. At WhiteSands, there are multiple group options throughout the course of the day, designed to fit the needs of individual patients based upon their background and history of use.
-
Individualized treatment planning
All patients will meet with their primary therapist within the first 24 hours of admission, to begin laying out your goals while in treatment. Detoxing from the substances you have been abusing is just the first step in your treatment at WhiteSands. We will also help you to identify and resolve any other issues in your life that may have led to or exacerbated your addiction.
-
Multiple individual sessions per week
All patients will be seen by their primary therapist a minimum of 2-3 times per week for individual sessions. This is an important distinction from the way a lot of treatment centers treat their patients. In most cases, you are seen by your primary therapist once per week, and the rest of the time you are in large group settings with the rest of the community. This does not allow for the deeper issues to be addressed and rectified while you are in treatment.
-
Family therapy
Family therapy is available and encouraged while in treatment. We offer these sessions either in person if your family lives locally or through video conference. Very often patients' loved ones and family do not have a full understanding of the disease of addiction, and it is through family therapy that we are able to educate and treat any existing family dynamics.
-
Family visitation is offered weekly or by special request
-
Smaller group sessions
Besides AA/NA meetings and community meetings, all of our groups are run with between 12-15 patients. This allows for more interaction and deeper processing of issues and occurs in daily process groups as well.
-
Licensed primary therapists
All of our primary therapists are licensed LCSW (licensed clinical social worker) or LMHC (licensed mental health counselor.)
-
Complete history and physical within the first 24 hours of admission to WhiteSands.
-
Extended slow tapers off of all mood and mind-altering substances
With the benefit of slow tapers, you are able to, but not mandated to attend group therapy from day 1. We understand there is an adjustment period for anyone entering treatment. Using a combination of controlled medications, our board certified Addictionologist will meet with you every day throughout the course of your detoxification, to both ensure you are as comfortable as possible, and make any necessary adjustments to your individualized protocol. Your safety and comfort are of the greatest importance to us through the detoxification process.
-
Licensed Nutritionist reviews and approves all menu options
-
Full-time dedicated staff
- Most of the treatment centers today employ part-time staff, particularly when it comes to medical and psychiatric staff, as a means of cutting costs and providing the minimum care possible to fall within compliance standards. While this is an effective means of saving money, it comes at the cost of patient care and one-on-one treatment.
- All of our staff are full-time employees of WhiteSands. We do not employ part-time employees who split their time between a number of treatment centers.
- We employ 3 board certified Addictionologists so patients will have access to these specialists 7 days a week.
- 24-hour nursing and support staff
Nursing staff, as well as community therapists, are on-site 24 hours a day, 7 days a week. Patients will be seen by our nursing staff for daily assessments throughout the course of their stay.
-
All vitals are monitored throughout the course of the day for your safety and comfort
-
Full psychiatric assessment within first 48 hours by Board Certified Psychiatrist
We employ 3 Board-Certified Psychiatrists who will work with you to identify and treat any underlying psychiatric issues that have not been addressed. Very often through medication management, these underlying psychiatric issues can be addressed effectively, so as to not impact your recovery going forward.
-
Follow up psychiatric assessments once a week
Why WhiteSands Does it Better
Why does WhiteSands do it better? Plainly said, WhiteSands was built with the goal to elevate the standards of care in addiction treatment, to ensure that we are giving patients the best chance at sustaining long-term sobriety and doing so in a safe and comfortable environment. I am Joe Ducey, the Chief Operating Officer of WhiteSands and someone who is in recovery. I wanted to build a treatment center that went to the next level in providing the best patient experience from the initial phone call to our admissions department until the day you complete our program.
It was with these guiding principles in mind when I approached my boss Garry Jonas (CEO of WhiteSands and a successful entrepreneur) to start WhiteSands. With his blessing and guidance, I got to work with our current Clinical Director, Lyndsay Henry, in researching all the treatment centers out there today, and the types of treatment currently available.
After an extensive amount of market research, exhaustive interviews to identify the best doctors, psychiatrists, therapists and nurses, and identifying properties conducive to recovery, WhiteSands officially opened its doors in March of 2013. Since then, we have treated over 10,000 patients struggling with both substance abuse and underlying psychiatric issues and have seen time and time again the success stories of those going through our programs. What follows is the WhiteSands difference, and how we have elevated standards of care for addiction treatment. You can be one of these success stories.
Some of the elements of how WhiteSands does it better:
-
Individualized treatment programs. At WhiteSands, we do not believe in a one-size-fits-all approach in anything we do. You will see this philosophy employed in both the programs and services we provide.
Compared to the average treatment center - Most treatment centers use a generic, one-size-fits-all approach to recovery that does not offer a personalized or individualized treatment plan.
-
Multiple one-on-one sessions with a licensed primary therapist. At WhiteSands you will meet with your primary therapist 4-5 times per week, allowing them the time to work on some of the deeper issues that have led you down the addiction path.
Compared to the average treatment center - The industry standards generally call for 1 individual session per week, which does not provide the time patients require for treatment to be effective.
-
Extended slow taper off of all mood and mind-altering drugs. Whether you are coming off of narcotic medication or alcohol, this can be a very uncomfortable and often dangerous process if not handled correctly. At WhiteSands, there should be no fear of the withdrawal process. Our board-certified Addictionologist will work with you one-on-one using extended tapers to wean you off the substance of choice, allowing you to get the maximum benefit of all the services we offer. We ensure that your detox experience is made as comfortable as possible.
Compared to the average treatment center - Compared to the average treatment center- Many facilities administer small doses of detox medications and only for 3-4 days, which results in a much less comfortable and more risky detox.
-
Board-Certified Addictionologist. An addictionologist will meet with you daily during the detoxification process. All of WhiteSands Medical staff are full-time employees, dedicated to helping you through the recovery process.
Compared to the average treatment center - Many facilities will not employ any addictionologists, or will hire them on a part-time basis, and will not have full-time doctors onsite. Many specialists that the average facility has, are employed by multiple centers. They simply make their rounds to each one, never building a personal relationship with the patient.
-
Dual diagnosis program with Board Certified Psychiatrist. These specialists are on-site 7 days per week. Every patient that comes to WhiteSands will be seen within 48 hours for a full psychiatric assessment, then will be seen once a week thereafter for follow-up evaluations and medication management.
Compared to the average treatment center - Standard treatment facilities do not have an on-site, full-time, board-certified psychiatrist but instead, hire them on a part-time basis.
-
Low patient-to-therapist ratio. At WhiteSands, we put a lot of focus on ensuring that there are no more than 10-12 patients in a group at any given time. It would certainly be less expensive to have much larger group sizes, thereby requiring less staff, but it is certainly not more effective. With low patient-to-therapist ratios, each patient can participate in a meaningful way in every group that they attend.
Compared to the average treatment center - In standard facilities, there are generally group sizes of 20 or more individuals. With this amount of people in a single group, there is simply no time for one-on-one interaction between the therapist and the patient, and groups essentially become a lecture.
-
State of the art recreation and athletic center. The theme at WhiteSands Treatment is that you are a patient from 8:30 am - 4:30 pm, and from 4:30 pm to 11:00 pm, you become a guest. Guests can relax and enjoy the amenities and can spend their free time exercising, partaking in activities and hobbies, or simply hang out in their private room where they can watch TV and stay connected with friends and family. We believe that having these features allows patients to absorb treatment better and, therefore, have a better chance at life-long recovery.
Compared to the average treatment center - Standard treatment centers offer very few, if any, recreational activities and amenities for patients to enjoy after treatment hours. This leaves patients bored and eager to get through treatment as quickly as possible so that they can get out.
A Testament to Our Success
AMA rates 10% below the industry average. In layman terms, AMA means leaving treatment against medical advice. A typical AMA rate for inpatient treatment centers is between 10 and 15% and generally indicates there are flaws within the program. At WhiteSands, our AMA rate is 4%, and the results speak for themselves, with thousands of people that have maintained long-term sobriety. WhiteSands success in this area can be attributed to our expertly trained staff who can talk you through those impulsive thoughts and decisions. This coupled with all of the amenities that we offer, is designed to make you much more comfortable while you are in treatment.
WhiteSands Alcohol & Drug Rehab - Florida


Please read our 10 point presentation below
Photo Gallery
Video Tour
Innovative Philosophies regarding Addiction Treatment
Amenities, Activities, Accommodations and Food
Patients are Treated as Guests at all Times When not in Treatment
- Overview
- 10-Acre Campus - Room to Breathe
- Private Rooms - Peace of Mind
- Cell Phones/Devices Allowed - Staying in Touch
- Brand New Recreation Center - Pass the Time
- Activities to Enjoy - Have Some Fun
- Newly Constructed Athletic Complex - More to do
- Fitness Programs and Personal Training - Get in Shape (Optional)
- Boxing Program - Blow off Steam (Optional)